by Charlotte Kilpatrick | Oct 11, 2024 | Global Health |
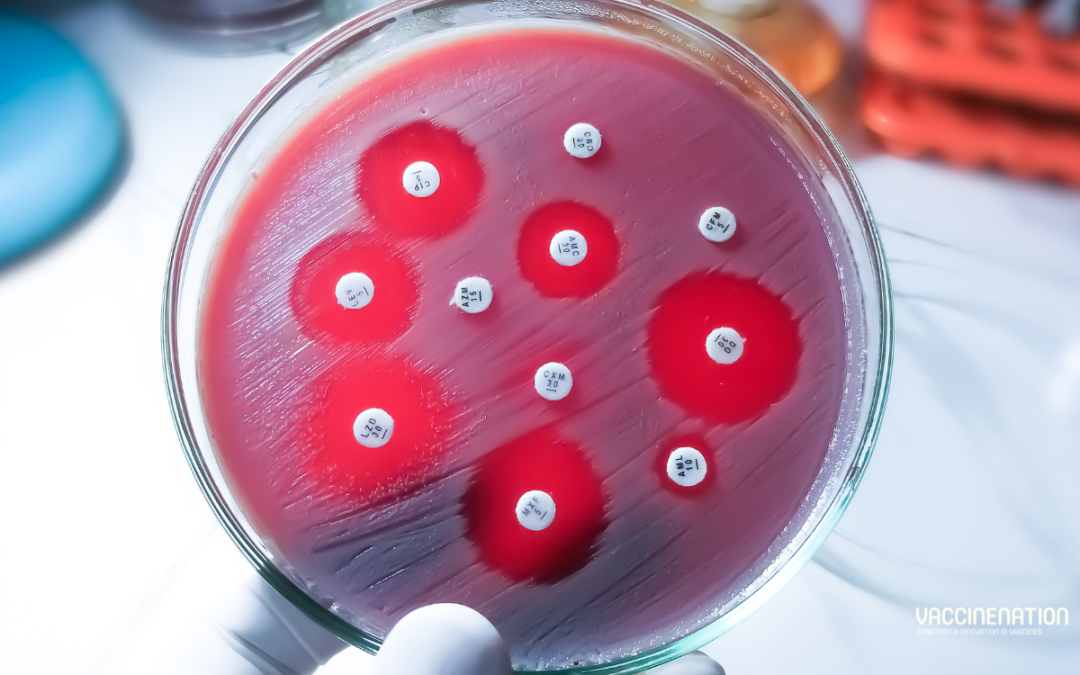
A WHO report in October 2024 suggests that vaccines against 24 pathogens could reduce the number of antibiotics needed by 22% every year. Some of these vaccines are already available but currently underused, but others will need to be developed and brought to market. The report expands on a WHO study from 2023, estimating that some vaccines already in use could avert up to 106,000 deaths caused by AMR each year. Director-General Dr Tedros Adhanom Ghebreyesus highlighted that addressing AMR “starts with preventing infections”, for which vaccines are “among the most powerful tools”.
“Prevention is better than cure and increasing access to existing vaccines and developing new ones for critical diseases, like tuberculosis, is critical to saving lives and turning the tide on AMR.”
The burden of AMR
Antimicrobial resistance (AMR) is the result of bacteria, viruses, fungi, and parasites changing to stop responding to medicines. As medicines become ineffective, infections become harder to treat, which increases the risk of disease spread, severe illness, disability, and death. The report introduces the significant global burden of AMR. In 2019, an estimated 7.7 million deaths were associated with 33 bacterial infections, with almost 5 million of these associated with AMR.
The mortality burden of these drug-resistant infections is “most pronounced” on the African continent, followed by South-East Asia and Eastern Europe. However, community mobility increases the risk of transmission to other continents. AMR has the potential to impose an annual global cost of up US$3.4 trillion by 2030, with the most severe consequences for low- and middle-income countries (LMICs).
A “key driver’ of AMR is the “systematic misuse and overuse” of antimicrobials in healthcare, animal health, and agriculture; the greatest contributor to overall use of antimicrobials is use in animals. The World Organisation for Animal Health (WOAH) estimated that 84,500 tonnes of antimicrobials were used in the animal sector in 2019. However, this is a 13% decrease from 2017. On the other hand, global antibiotic consumption in humans increase by 65% between 2000 and 2015 and is projected to triple (from 2015) by 2030.
One of the major challenges is ensuring equitable access to antimicrobials, particularly in LMICs, where “people are more at risk of dying from a lack of access to appropriate antimicrobials than from resistant infections”. Managing AMR demands both sector-specific and “One Health” approaches. Vaccines can be critical to efforts to lower the burden by reducing the incidence of drug-sensitive and drug-resistant infections, antibiotic use, and opportunities for evolution and transmission of resistant genes and pathogens.
The report
Although we know that vaccines are important aspects of the solution, their specific role in reducing AMR has not been “systematically evaluated and quantified”. Therefore, the latest report evaluates this and provides recommendations for “enhancing the impact of vaccines on AMR”. It covers 44 vaccines targeting 24 pathogens, drawing the characteristics of each vaccine from various sources. Three criteria were considered:
- The AMR-related health burden – measured by the reduction in deaths and DALYs associated with AMR
- Antibiotic use (or antimicrobial use in the case of Mycobacterium tuberculosis)
- The economic burden of AMR, including hospital costs and productivity losses
Highlights from the report
- Vaccines against 16 bacterial pathogens may prevent 510,000 deaths and 28 million DALYs associated with AMR.
- This prediction increases to include an additional 1.2 million deaths and 37 million DALYs when the use of vaccines is expanded to target all populations at risk of infection.
- The non-serotypespecific vaccine against S. pneumoniae, with increased efficacy against lower respiratory tract infections, would have the highest impact on both AMR-associated deaths and DALYs.
- The greatest impact of vaccines on reducing the burden of bacterial AMR in 2019 was in the WHO African Region, averting an estimated 170,000 deaths and 12 million DALYs annually.
- In the WHO South-East Asia Region, vaccines were estimated to have prevented 160,000 deaths and 7.5 million DALYs annually.
- The development and optimal use of vaccines against 23 pathogens could avert up to 2.5 billion defined daily doses a year, which is 22% of the global estimated antibiotic use in humans associated with treating these pathogens.
What’s next?
The authors suggest that the role of vaccines in addressing AMR is “often overlooked” in policy and decision-making processes. They highlight the need for “greater recognition and integration” of vaccines into AMR mitigation strategies and the importance of considering AMR in vaccine decision-making.
“To achieve appropriate inclusion of vaccines in the AMR agenda, the immunisation and AMR communities must strengthen their joint understanding of the evidence and enhance collaboration.”
How do you think that AMR priorities can be incorporated into vaccine development and deployment efforts? Join us for the AMR and bacterial vaccines track at the Congress in Barcelona this month to contribute to these conversations, and don’t forget to subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Sep 23, 2024 | Technology |
Evaxion Biotech announced the launch of an enhanced version of its clinically validated AI-Immunology platform in September 2024, with an update to the EDEN AI prediction model. Improvements to the model include toxin antigen prediction, which enables the development of improved bacterial vaccines. AI-Immunology allows Evaxion to simulate the immune system and create predictive models to identify and develop personalised and other next-generation immunotherapies. It uses advanced AI and machine learning technologies to design and develop vaccine candidates in response to significant unmet needs.
EDEN upgraded
The AI-Immunology platform can deliver a new target within 24 hours, with “robustly validated” predictive capabilities. The EDEN prediction model is one of five models within the AI-Immunology platform. It rapidly identifies antigens that will trigger a robust protective immune response against “almost any” bacterial infectious disease. The model is fully AI-driven and designed to identify vaccine candidates “faster and at a lower cost than current state-of-the-art methods”. EDEN enables a novel approach to vaccine development that supports efforts against the “rising global issue of antibiotic resistance”.
The latest version 5.0 features several updates:
- Novel bacterial toxin antigen predictor – Evaxion has trained new machine learning models to improve the accuracy and reliability of toxin antigen prediction.
- Expanded training dataset – The process for curating additional training data from published sources has been streamlined with retrieval-augmented generation with large language models, followed by manual domain expert curation.
- Advanced protein feature prediction – The team has developed a new building block for protein feature prediction using protein language models, enhancing the model’s architecture and capability to predict various protein characteristics.
CEO of Evaxion, Christian Kanstrup, described the launch of the model as an “important milestone” that strengthens the AI-Immunology platform.
“As one of the few truly AI-first TechBio companies, our AI-Immunology platform is at the forefront of innovation. We wil continue to invest in its development and refinement to further improve our ability to discover novel targets and develop advanced vaccines.”
We look forward to learning more about the AI-Immunology platform at the Congress in Barcelona next month; get your tickets to join us there and don’t forget to subscribe to our weekly newsletters for more vaccine technology updates.

by Charlotte Kilpatrick | Sep 6, 2024 | Global Health |
The Vaccine Group (TVG) announced in September 2024 that its partnership with the University of Plymouth and the University of Cambridge has been awarded “significant” government funding to develop a vaccine to stop the development and spread of Streptococcus suis. Streptococcus suis is a bacterial infection that commonly affects the UK pig population. It can cause serious disease in pigs and has the potential to infect the humans working with them.
Streptococcus suis
Affecting more than 60% of pig farms across several countries in Europe, Streptococcus suis threatens both the pork industry and public health. It is a “noteworthy” pathogen responsible for significant bacterial mortality in piglets after weaning. There are no proven vaccines to address the disease’s “many strains”, and infected pigs are treated with different antibiotics.
The UK Government is targeting a 50% reduction in antibiotic use in livestock by 2030, so TVG is responding to the urgent demand for an effective vaccine. Their project will assess if a vaccine candidate that is already effective against the most common strain of the disease can protect pigs against multiple, or all, known strains. This has potential to also prevent transmission to humans.
DEFRA’s Farming Innovation Programme is providing a grant of over £1 million through Innovate UK. The project will unite experts from vaccine development, antimicrobial resistance, and veterinary medicine; it develops previous research that identified the potential candidate for the Streptococcus suis vaccine. Trials will be carried out with Moredun Scientific Ltd to explore the vaccine’s potential. The team will engage the pig farming community in their research to ensure that the vaccine meets requirements and can be administered in an “efficient and cost-effective manner”.
Dr Jeremy Salt, CEO at The Vaccine Group, described Streptococcus suis as a “major cause for concern” for farmers across the UK. It can lead to “significant losses”. Furthermore, as a zoonotic infection, it presents a risk of transmission to humans in the industry.
“Our goal in developing an effective vaccine is to stop the bacterial infection from developing in pigs and humans in the first place. By doing so, we can better protect the farmers, their animals, and their livelihoods.”
Dr Salt also hopes to make pork production “more efficient, human, and sustainable”, whilst helping the sector “address the global challenges of antibiotic resistance and carbon emissions”.
We look forward to welcoming Dr Salt back to the Congress in Barcelona to chair our One Health and Veterinary Track; get your tickets to join us there, and don’t forget to subscribe to our weekly newsletters for vaccine updates.

by Charlotte Kilpatrick | Aug 21, 2024 | Global Health |
A report shared by Africa CDC in August 2024 finds that the threat presented by treatment-resistant diseases has increased in Africa, with children and other vulnerable groups at greatest risk. African Union AMR Landmark Report: Voicing African Priorities on the Active Pandemic, demands a “comprehensive, multi-sectoral approach involving the entire society” to address the challenges of antimicrobial resistance (AMR), which extend beyond morbidity and mortality.
“The comprehensive measures outlined in this report are essential for curbing the threat of AMR in Africa, ensuring the health and prosperity of future generations, and achieving sustainable development goals across the continent.”
The global and continental burden
The authors describe the “existential impacts” of AMR as “far-reaching”; it represents a “significant public health challenge”. 4.95 million deaths in 2019 were associated with bacterial AMR, of which 1.27 million deaths were “directly attributable” to AMR, surpassing the burden of HIV and malaria. This highlights that AMR is a leading cause of mortality, but sub-Saharan Africa suffers greatest burden. Beyond death and disability, AMR “carries substantial economic implications at personal, national, and global levels”. AMR is projected to result in an additional US$1 trillion in healthcare expenses by 2050.
The report acknowledges that antibiotics are considered the “cornerstone of modern medicine”. However, the emergence and re-emergence of AMR could “potentially revert us to an era when antibiotics did not exist”.
“AMR not only threatens to roll back decades of development gains and disrupt healthcare services but also poses a significant barrier to achieving global health security and economic development.”
The highest burden of AMR is in low-resource settings, which have the greatest infectious disease burden and “weaker” health systems. In 2019, sub-Saharan Africa (SSA) experienced the highest rate of AMR burden; 23.7 deaths per 100,000 people and 255,000 deaths were attributed to AMR. Notably, this surpasses malaria and HIV/AIDS mortality.
Although The World Health Assembly adopted the Global Action Plan on AMR, endorsed in the 2016 UNGA high-level meeting on AMR, the adoption and implementation of AMR interventions in Africa is “limited”. This is attributed to “misalignment of priorities, lack of resources, and inadequate coordination”. Thus, the imminent UNGA high-level meeting on AMR offers Africa the opportunity to “elevate its priorities and secure commitments” to address the challenge.
Implementation of AMR One Health National Action Plans (NAPs) has had “mixed” progress. The report suggests that this has been “fragmented” due to dependence on foreign funders and a “lack of awareness, knowledge, and appreciation” of the threat. However, the authors recognise “commendable progress in certain areas”. For example, Africa has made “significant strides in stewardship and surveillance”; 57% of African countries have adopted the AWaRE (Access, Watch, Reverse) classification of antibiotics on National Essential Medicine Lists (NEMLs). 50% of African countries have implemented integrated surveillance systems for AMR. These improvements, though slow, highlight “potential and ongoing efforts”.
A key challenge is access to antibiotics, with “many” countries relying on imports for over 90% of their pharmaceutical needs. This results in “frequent shortages and chronic out-of-stocks”. Additionally, global supply chain pressures can affect access in LMICs and undermine the resilience of health systems. Lack of access leads to over-reliance on the few available drugs, even if they are not the primary choice, and can result in “severe health outcomes”.
The registration process for some antibiotics is lengthy, which discourages pharmaceutical companies from entering and limits the availability of essential medicines. Furthermore, continental investment in research and development is “inadequate”; “very few countries” have the infrastructure for Phase III clinical trials and local data on AMR remain “insufficient”.
“By aligning African needs with global efforts, the continent can effectively enhance its capacity to combat AMR and contribute to the global response.”
The challenges
The effort required to address AMR in Africa faces “specific challenges”:
- Strengthening governance and leadership – governance and coordination structures are still not completely aligned with the frameworks outlined in the Global Action and National Action Plans. This misalignment creates gaps in integrating diverse stakeholders and sectors and hinders accountability.
- Addressing the driver of AMR in Africa – addressing the drivers of AMR in Africa involves tackling multiple contributing issues. These include gaps in IPC/WASH programmes, poor adherence to biosecurity and animal husbandry practices, vaccination challenges, regulatory barriers, socio-economic barriers, low public awareness, and underdeveloped public health systems.
- Building evidence and improving reporting – understanding the landscape and responding with informed decisions requires robust evidence and effective reporting systems. Data collection, analysis, and utilisation systems are often inadequate, with only a few comprehensive AMR surveillance systems. A lack of standardised reporting mechanisms and integration of surveillance data across human, animal, and environmental health sectors hinder the creation of a cohesive evidence base.
- Mobilising and coordinating resource effectively – the continent often depends on sporadic international funding, which leads to fragmented efforts and short-term projects that neglect the enduring nature of AMR threats. Lack of sustained financial commitment undermines the continuity and effectiveness of AMR control measures.
- Strengthening community engagement and education – gaps in community engagement and education limit public understanding and support for initiatives. Without comprehensive community involvement and educational outreach, efforts to encourage responsible antimicrobial use and enhance infection prevention and control measures are weakened.
- Enhancing research and innovation – progress is hampered by various obstacles such as limited funding, inadequate infrastructure, and a shortage of skilled researchers. Development and implementation of solutions is also hindered by lack of collaboration between institutions and restricted access to advanced technologies.
Priority actions
The report offers the following priority actions in response to these challenges:
- Enhance leadership commitment, implement integrated governance structures, strengthen coordination and communication, define clear terms of reference, promote legislative support and institutional mechanisms, engage diverse stakeholders.
- Improve adoption of IPC, WASH, biosecurity, and animal husbandry measure in human, animal, and environmental sectors, increase vaccination rates for high-priority pathogens in high-risk African countries, raise public, professional, and policymaker awareness of AMR, increase uptake of alternatives to antimicrobials, increase availability of high-quality diagnostics, vaccines, and antimicrobials for high-priority pathogens in high-risk African countries.
- Establish country-level baselines for antimicrobial consumption and resistance, consolidating country-wide reporting, define a core set of indicators to measure the impact of AMR in Africa, measure the cost of inaction in the African context, strengthen data and information sharing platforms.
- Endorse targets applicable for Africa to support AMR actions, mobilise funding to close the gap for AMR actions across Africa, support fully costed NAPs with funding tied to milestones, promote the One Health approach by incorporating AMR into broader agendas to coordinate resources.
- Develop and implement comprehensive public education campaigns, enhance community-based interventions, strengthen pre-service-based education programmes, facilitate professional development and training, leverage technology and social media.
- Increase funding and investment in research, build and upgrade research infrastructure, promote interdisciplinary and cross-sector collaboration, streamline regulatory and ethical approval processes, support capacity building and talent retention.
Goals and conclusions
The short-term goals (0-6 months) focus on sharing the report with stakeholders and engaging these stakeholders to discuss recommendations, build consensus, and refine strategies for implementation. Medium-term goals (6-12 months) place an emphasis on key policy recommendations, including establishing “robust” regulatory frameworks, launching public awareness campaigns, and developing and strengthening surveillance systems.
“These efforts will involve significant investments in capacity building, technology upgrades, and the establishment of data-sharing protocols across countries and regions.”
Long-term goals (12+ months) focus on monitoring and evaluating progress, with assessments against the core objectives of the Global Action Plan (GAP) on AMR. This phase also involves “sustained efforts” to mobilise financial, technical, and human resources to support ongoing and new initiatives.
“Strengthening partnerships with international donors, private sector stakeholders, and regional bodies will be crucial to ensuring the continued availability of resources and support.”
The authors conclude the report by looking forward to the UNGA high-level meeting on AMR and reminding stakeholders of the importance of uniting in support of the recommendations. They highlight the significance of collaboration to implement the strategies and ensure progress is sustainable.
“The stakes are high, and the potential benefits of addressing AMR are immense. Investing in AMR initiatives will save lives, improve health outcomes, boost economic productivity, and strengthen healthcare systems across the continent. We call upon the global community to recognise the urgency of the AMR crisis in Africa and commit to taking bold and coordinated actions.”
Comments
Africa CDC Deputy Director General Dr Raji Tajudeen, speaking at the launch of the report, commented that the “silent threat” of AMR must not be ignored.
“Fighting disease requires resources and working with member states and our partners; we need to do all we can to save lives.”
Dr Huyam Salih, director of the African Union-Inter African Bureau for Animal Resources (AU-IBAR), drew attention to the fact that AMR is “not just a health issue”.
“It is a threat to our agrifood systems, food safety, food security, livelihoods, and economies.”
This is “particularly alarming” in Africa, where 37 countries report the prevalence of AMR in animal farms, but on 16% of countries are conducting routine AMR surveillance in animals.
“Our health, our food, and our future depend on the actions we take now.”
Nqobile Ndlovu, head of the African Society for Laboratory Medicine, emphasised the organisation’s commitment to strengthening laboratory capacities to address AMR.
“Our goal is to ensure the continued efficacy of treatments and promote data-driven solutions to safeguard public health across the continent.”
For more on the role that vaccines can play in global efforts against AMR, why not join us at the Congress in Barcelona this October? Get your tickets here and don’t forget to subscribe to our weekly newsletters here. You can also check out our Congress interview from Washington with Dr Yewande Alimi, who led and wrote the report, for her insights into AMR in Africa.

by Charlotte Kilpatrick | Aug 19, 2024 | Global Health |
In August 2024 the Pan American Health Organisation (PAHO) and the Latin American Society of Paediatric Infectious Diseases (SLIPE) signed a cooperation agreement with the aim of reducing infectious diseases prevalent among children and adolescents in Latin America. Although deaths in children under 5 years have decreased by 60% in Latin America and the Caribbean since 2000, infectious diseases continue to represent a major health threat to the age group.
“In addition to causing mortality and disability, these diseases impose significant economic and social costs on families and communities, disproportionately affecting those with limited resources and in vulnerable situations.”
A 5-year framework
The agreement is a 5-year, renewable technical cooperation framework agreement and aligns with PAHO’s initiatives to address infectious diseases and promote child and adolescent health in the region. PAHO and SLIPE will work together on projects in “key areas” such as vaccination, paediatric infectious diseases, arboviruses, perinatal infections, and neonatal sepsis. They will also collaborate on efforts to “strengthen surveillance systems, promote ongoing research to inform clinical practices, and implement awareness campaigns”.
Dr Alfonso Tenorio Gnecco, PAHO/WHO Representative in Costa Rica signed the agreement on behalf of PAHO Director Dr Jarbas Barbosa and hopes that it will enable PAHO to “provide technical and strategic guidance to strengthen health systems and address childhood infections”.
“Our goal is to reduce preventable child deaths through a comprehensive range of interventions.”
SLIPE President Dr María Luisa Ávila described the signing as a “crucial step in the fight against antimicrobial resistance in the region”.
“This collaboration will enhance our capacity to tackle this growing threat by promoting joint actions and implementing our strategies based on scientific evidence, which are essential for protecting the health of our children and adolescents in Latin America.”
To join discussions about infectious disease management and global health goals at the Congress in Barcelona this October, get your tickets here, and don’t forget to subscribe for weekly insights here.

by Charlotte Kilpatrick | Aug 16, 2024 | Infection |
Data from the UK Health Security Agency (UKHSA) shared in August 2024 reveals a “concerning rise” in antibiotic-resistant gonorrhoea infections in England. In 2023 over 85,000 gonorrhoea diagnoses were reported in England; this is the highest number since records began in 1918. There were also 15 confirmed cases of infection with ceftriaxone-resistant Neisseria gonorrhoeae detected in England between June 2022 and May 2024. Since the initial case detected in England in 2015, there have been a total of 31 ceftriaxone-resistant Neisseria gonorrhoeae cases. UKHSA highlights the importance of “regular” STI testing, particularly for people who have “condomless sex with new or casual partners”.
Developing resistance
Gonorrhoea is the second most commonly diagnosed sexually transmitted infection (STI) in England. In 2023 the highest annual number of diagnoses (85,223) since records began was reported. The bacteria, Neisseria gonorrhoeae, has developed resistance to every class of antibiotics used to treat it. Cephalosporins are the last remaining class of antibiotics available for use as empirical monotherapy. The recommended first-line therapy is 1g ceftriaxone (a cephalosporin), but there are “sporadic” cases of infection with ceftriaxone-resistant N. gonorrhoeae.
16 cases were reported between 2015 and May 2022; since then, a further 15 ceftriaxone-resistant infections have been detected in England. Five of these recent cases were extensively drug-resistant (XDR). All 31 cases detected in England have been among heterosexual individuals, mostly in their 20s, and “most” have acquired infection in the Asia-Pacific region, which is the region with the highest prevalence of ceftriaxone-resistance.
UKHSA response
UKHSA has sent a clinical alert to sexual health services to “reinforce the need” to culture gonococcal isolates, perform test-of-cure, and refer all ceftriaxone-resistant N. gonorrhoeae strains or potential treatment failures to UKHSA. It also emphasises the importance of correct and consistent condom use to the public.
Dr Helen Fifer, Consultant Microbiologist at UKHSA, highlighted a concern that gonorrhoea could become “untreatable” in the future.
“Untreated gonorrhoea can lead to serious health issues, including pelvic inflammatory disease and infertility. Condoms are the best defence, but if you didn’t use one with a recent new or casual partner, get tested to detect the infection and prevent onwards transmission.”
Professor Matt Phillips, President of the British Association for Sexual Health and HIV (BASHH) described the rise of these antibiotic-resistant infections as a “worrying trend” that “must be addressed with immediate action”.
“Antibiotic resistance of STIs poses an increasingly major public health threat, which can create physical and psychological harms and place additional demands on other parts of the NHS.”
Professor Phillips stated that BASHH and sector partners have “repeatedly called” for a sexual health strategy for England.
“This must be a priority if our expert sexual health workforce are to effectively meet these growing and changing needs in sexual health.”
In January 2024 CARB-X announced funding for Intravacc’s vaccine efforts against gonorrhoea, which you can read about here. We also look forward to further exploring the role of vaccines in addressing the growing challenge of N. gonorrhoeae at the Congress in Barcelona this October, so get your tickets to join us there, and don’t forget to subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Jul 9, 2024 | Global Health |
A study in JCI Insight in July 2024 presents work from researchers at Trinity College Dublin who sought to improve vaccine responses to Staphylococcus aureus. The “potentially deadly bacterium” induces IL-10, which “impedes effector T cell responses” to allow persistence during colonisation and infection. In the study, IL-10 expression was elevated in the nares of persistent carriers of S. aureus, which was associated with reduced systemic S. aureus-specific Th1 responses. From this, the authors infer that systemic responses are remodelled through commensal exposure to S. aureus, negatively affecting vaccine function. They found that blocking IL-10 during vaccination enhanced T cell responses and improved bacterial clearance in subsequent systemic and subcutaneous infection, possibly indicating a novel strategy for improved efficacy.
An urgent need for effective interventions
S. aureus is a leading cause of both community-acquired and hospital-acquired bacterial infections and is associated with more than 1 million deaths each year. Although it is a major source of fatal bloodstream infections, the most common manifestations of infections are chronic and recurrent skin and soft tissues infections (SSTIs). Treatment of staphylococcal infections is “increasingly challenging” in the face of antimicrobial resistance (AMR), and S. aureus is the leading cause of AMR deaths in high-income countries.
“The health risk posed by S. aureus infection urgently necessitates the development of novel effective therapies that improve clinical outcomes by providing broad-spectrum protection, regardless of antimicrobial resistance patterns. The development of an efficacious, prophylactic anti-S. aureus vaccine is now more urgent than ever, as treatment options narrow further.”
Despite “significant” efforts over recent decades, there is no effective vaccine against S. aureus infection. Antibody-based vaccination strategies are “not working” and effective vaccines will need to induce protective cellular as well as humoral immunity.
The role of the microbiota in vaccine-induced immune responses is becoming more appreciated as the association between the composition of the infant microbiota and immune responses to vaccination is reported in more studies. The microbiota can negatively influence vaccine efficacy and has been reported to inhibit BCG-induced protection against Mycobacterium tuberculosis infection by “skewing” vaccine-induced immunity in favour of suppressive Tregs (regulatory T cells). Data suggest that exposure to organisms with capacity to drive immunosuppression can “interfere” with vaccine-induced effector responses.
In the context of S. aureus, research suggests that exposure could “imprint” the immune system in a suppressive manner. Therefore, past exposure could affect the ability of vaccines to drive protective T cells responses during subsequent infection. In nasal colonisation and skin infection, S. aureus drives local production of the immunosuppressive cytokine IL-10 to dampen effector T cell responses and facilitate bacterial persistence. The researchers believe that, if there is an immunosuppressive imprint that interferes with vaccine-induced T cell function, inhibition of anti-inflammatory immune responses during vaccination could be a way of enhancing vaccine efficacy.
The study
“This study reveals a potential bottleneck that may need to be circumvented to realise an effective vaccine.”
The researchers demonstrate that S. aureus colonisation drives the production of IL-10 in the nasal cavity of healthy adults, likely to facilitate bacterial persistence. This is associated with “altered circulating memory T cell responses” when exposed to S. aureus antigens. In preclinical models, they demonstrate that the transient inhibition of IL-10 during immunisation improved vaccine-induced T cell responses to lead to a more effective clearance of infection. This approach was more effective when the vaccine was administered with adjuvants to drive antigen-specific Th1/Th17 responses.
“This study supports the premise that colonisation status has a direct impact upon system S. aureus-specific memory T cell responses, which could be hindering vaccine function due to the promotion of an immunosuppressive state.”
After offering insight into the “critical role” that IL-10 plays in “impeding” anti-S. aureus vaccine efficacy by “dampening” vaccine-induced protective T cells responses, the authors propose a method of improving vaccine efficacy by inhibiting IL-10 production during vaccination. This leads to enhanced antigen-specific T cell responses and improved bacterial clearance.
Professor Rachel McLoughlin at Trinity College Dublin’s School of Biochemistry and Immunology led the research team and believes that their results “offer significant promise for what would be a novel strategy for improving the efficacy of vaccines developed with the aim of suppressive S. aureus infection”.
“Our work also strongly suggests that prior exposures to this bacterium may create a situation whereby our immune system no longer sees it as a threat and thus does not respond appropriately to a vaccine due to the creation of this immune-suppressed state. Again, this underlines why immunisation delivered with something that helps neutralise IL-10 offers renewed hope for effective vaccines against S. aureus.”
For more updates on developing vaccine strategies to deadly infectious diseases, why not join us at the Congress in Barcelona this October? Don’t forget to subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Jun 19, 2024 | Global Health |
A paper in Vaccine in June 2024 considers how vaccines can be used to reduce the growing threat of antimicrobial resistance (AMR). The authors suggest that, although vaccines can avert drug-sensitive and resistant infection, reduce antibiotic usage, and lower the likelihood of developing resistance genes, the role of vaccines in mitigating AMR is “currently underutilised”. They use previous research that utilises Vaccine Value Profiles to inform vaccine development and analyse the effects of 16 pathogens.
A “significant global burden”
Antimicrobial resistance (AMR) “poses a significant global burden”; estimates indicate that approximately 4.95 million deaths globally were associated with bacterial AMR in 2019. Many of these occurred in low- and middle-income countries, which are “particularly vulnerable” to the spread of AMR because of factors like “poor water and sanitation infrastructure, limited access to healthcare including diagnostics and effective treatments, and misuse and overuse of antibiotics”.
Vaccines can play a critical role in preventing AMR through “several mechanisms”:
- Vaccines reduce the incidence of infections with drug-susceptible and drug-resistant pathogens, leading to a reduction in cases, deaths, and economic costs.
- Vaccines can prevent secondary infections.
- If enough people are vaccinated, vaccines protect both individuals and communities through herd immunity.
- When infections are prevented by vaccines, the use of antibiotics decreases.
“Despite the clear mechanisms by which vaccines can impact AMR, vaccines are too often overlooked in the medical and popular literature as powerful tools to reduce AMR, especially in concert with other interventions such as effective sanitation, hygiene, and infection prevention measures, antibiotic access and stewardship measures to optimise use, and continued efforts to develop new antimicrobial agents.”
WHO’s Action Framework to leverage vaccines against AMR and antibiotic use is centred around three strategic goals:
- Expand use of licensed vaccines to maximise impact on AMR
- Develop new vaccines that contribute to prevention and control of AMR
- Expand and share knowledge of vaccine impact on AMR to help advocate for further investment
The authors call for acceleration of the development of vaccines for pathogens with “high potential for impact on AMR” to effectively control transmission. However, they recognise “several challenges” in vaccine development, including “diversity of vaccine-targeted populations, the complexity of vaccine biology, and the high degree of genetic diversity among pathogen strains, as well as the lack of clarity about their impact”. Thus, it is “essential” to expand knowledge of the potential impact of vaccines and other tools and to continue investing in their development.
“Combining vaccines with other prevention and control strategies such as improved sanitation and hygiene, as well as optimising the use of antimicrobial medicines, control of disease transmission through vector control and behavioural changes is required to effectively curb the spread of AMR.”
Another conclusion is that multi-pathogen combination vaccines could “play a role” through single administration and potential to “specifically target the primary pathogens responsible for distinct clinical syndromes”.
To see the full report of the 16 pathogens, click here. AMR returns to the agenda for this year’s Congress in Barcelona, so don’t forget to get your tickets to join us and subscribe for more insights.

by Charlotte Kilpatrick | May 29, 2024 | Technology |
In May 2024, the University of Saskatchewan (USask) shared that a research team from Western College of Veterinary Medicine (WCVM) has developed an aerosol vaccine that is “proving effective” in providing protection for young broiler chicks against necrotic enteritis. This is described as a “deadly disease” for poultry and a One Health issue that affects both animals and humans.
Necrotic enteritis
Necrotic enteritis is caused by intestinal overgrowth of Clostridium perfringens type G in poultry, reportedly contributing to a 50% fatality rate in affected chickens and “numerous” food poisoning cases in people. Dr Hemlata Gautam suggests that the disease is “basically re-emerging” because of “less use of antibiotics” in the poultry industry. Dr Gautum, under the supervision of WCVM’s Dr Susantha Gomis, is investigating “alternative strategies” for controlling and preventing the spread of necrotic enteritis without antibiotics.
Turning away from prophylactic antibiotics
Although antibiotics have been “instrumental” in the prevention of disease, the poultry industry in Canada is “phasing out” prophylactic use of antibiotic drugs in broiler chicken production in response to “overuse and the spread of antimicrobial resistance”. Dr Gautam highlights that there is “no effective control” of the disease at the moment.
“Scientists are working toward finding a preventative strategy. In my research, we have developed a vaccination strategy to prevent this disease.”
The strategy
The new strategy involves making chickens “strong enough to fight infection by the third week” of life, working around maternal antibodies and weak immune systems. Therefore, the strategy must begin very early in the chickens’ lives. In study, Dr Gautam injected synthetic DNA into the eggs just before the birds hatched, to help activate their immune systems. Through the concept of mucosal vaccination, she relied on the “gut-lung axis” to deliver the vaccine.
After the chicks hatch, they are placed in a special nebuliser to receive a single dose of a live, aerosol vaccine through the lungs. At three weeks, Dr Gautam exposed the chicks to Clostridium perfringens for three days. She found that the vaccinated birds had “completely healthy” intestines.
“What we have found is just by giving [chicks] one single vaccine dose by the lungs, we are able to protect them against necrotic enteritis.”
Although these results are positive, Dr Gautam reflects that the vaccine has only been used in experimental trials.
“To say completely how it will work in field conditions, we’ll have to do some field trials.”
However, she is encouraged by its potential and hopes that a similar strategy could be used against other infectious diseases in poultry.
“It’s a growing area right now – how we can give vaccines in the lungs and how it can protect different areas of the intestine. This [vaccination] strategy might be helpful for other infectious diseases as well.”
For more on technology for global health issues don’t forget to subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | May 21, 2024 | Infection |
A WHO report shared in May 2024 details the continued “significant public health challenges” posed by HIV, viral hepatitis epidemics, and sexually transmitted infections (STIs). The report identifies increasing cases of STIs across “many regions”, flagging “threats to the attainment” of targets outlined in the Sustainable Development Goals (SDGs) for 2030. The report is the first in a series of biannual progress reports on implementation of global health sector strategies for the period 2022-2030.
Infections increase
WHO states that four curable STIs – syphilis (Treponema pallidum), gonorrhoea (Neisseria gonorrhoeae), chlamydia (Chlamydia trachomatis), and trichomoniasis (Trichomonas vaginalis) – account for “over 1 million infections daily”. A reduction of 20% in these four infections must be achieved to realise targets by 2025 and a reduction of 60% is needed for the 2030 targets.
“The available data suggest that the world is off track to meet targets, with increasing rather than declining trends in new infections.”
Syphilis case increases have been driven by an “increase in the number of estimated new cases of syphilis in the WHO African Region and the WHO Region of the Americas”. These regions regularly share data within the Global AIDS Monitoring process. The report identifies “unprecedented high levels of new infections”, demanding an “urgent acceleration of efforts”.
The data also suggest an increase in “multi-resistant gonorrhoea”. By 2023, from the 87 countries with enhanced gonorrhoea antimicrobial resistance surveillance, 9 countries reported elevated levels.
HIV and hepatitis B challenges
The report suggests that “key achievements demonstrate the feasibility of ending AIDS as a public health concern by 2030. However, “many challenges remain”. For example, in 27 low- and middle-income countries, “less than 50% of people living with HIV were receiving antiretroviral therapy” in 2022. The current rate of declining incidence and HIV-related deaths is “insufficient” to achieve 2025 targets. Furthermore, children under 15 are bearing a “disproportionate burden of mortality”, reflecting “policy and programmatic failings”.
Viral hepatitis is “one of the leading infectious causes of death worldwide”, despite interventions that would support elimination of hepatitis B virus and hepatitis C virus by 2030. These include effective hepatitis B vaccines and effective treatments.
“Access to prevention, testing, and treatment remains low, resulting in increasing mortality and large numbers of new infections…Regaining the trajectory will require strengthening political will and mobilising greater investment.”
Major concerns
Dr Tedros Adhanom Ghebreyesus, WHO Director-General, finds “major concerns” in the rising incidence of syphilis.
“We have the tools required to end these epidemics as public health threats by 2030, but we now need to ensure that, in the context of an increasingly complex world, countries do all they can to achieve the ambitious targets they set themselves.”
Dr Meg Doherty, Director of the Department of Global HIV, Hepatitis, and Sexually Transmitted Infections Programmes at WHO, commented that there has been “impressive uptake” of WHO policies and “expansion of service access”. This is “particularly notable for HIV testing and antiretroviral therapy coverage” alongside expansion of hepatitis C treatment in a “small number of countries”. However, “many challenges persist”.
“While working to further expand services, especially for viral hepatitis and sexually transmitted infections, countries also must prioritise person-centred approaches and sustainability planning across all disease areas, focusing on political commitment, programmatic integration, and financing, while combatting stigma and discrimination in healthcare settings.”
To read the full report, click here. Don’t forget to subscribe to our weekly newsletters for infectious disease updates and insights into vaccines for global health goals.

by Charlotte Kilpatrick | May 17, 2024 | Global Health |
In May 2024 the UK Government announced that it will commit up to £85 million to the “growing threat” of antimicrobial resistance (AMR). At an event hosted by the Royal Society, global leaders came together to agree actions for tackling AMR and to hear accounts from AMR survivors. In the same week, WHO released the updated Bacterial Priority Pathogens List (BPPL) 2024, which features 15 families of antibiotic-resistant bacteria for prioritisation.
UK investments
The following initiatives were announced by the government:
- Up to £50 million to partner with countries in Africa to improve access to essential antimicrobial drugs, building on work by the UK Global AMR Innovation Fund and local expertise.
- Up to £25 million including partnering with countries and territories in the Caribbean to strengthen AMR surveillance systems and enable accurate monitoring of threats, through regional partners such as the Caribbean Public Health Agency and PAHO. This builds on the existing investment in the Fleming Centre in London and will allow the government to explore how to support the delivery of AMR centres in alignment with the Fleming Initiative.
- Up to £10 million over 5 years to help establish a global independent scientific panel for AMR, modelled on the success of other international panels such as the Intergovernmental Panel on Climate Change (IPCC).
- Alongside these programmes, £1.8 million has been allocated to the creation of a dedicated team in MHRA to support creating novel antimicrobials and diagnostics.
The projects “build on ongoing international and domestic work” to prevent the spread of AMR. Health Minister Andrew Stephenson commented that AMR is a “threat the world must take extremely seriously” and could “render our most vital medicines useless”. UKHSA reports that in 2019 4.95 million global deaths were associated with drug-resistant bacterial infections. By 2050 this is set to rise to 10 million, and the global economic cost of this is calculated to be $100 trillion.
The Foreign Secretary, Lord Cameron, identified AMR as a “global emergency posing a vast threat to our health, our development, and our security”.
“We must do more to tackle this threat and do it together, because it is too big to tackle without united global action.”
Jeremy Hunt, Chancellor of the Exchequer, is “deeply concerned” about the threat AMR poses “not just to the UK but to the world”.
‘The COVID-19 pandemic was conclusive proof that health emergencies don’t respect borders. That’s why I’m proud that the UK continues to play a pivotal role in bringing countries together to tackle emerging global health threats.”
UK Special Envoy on AMR, Dame Sally Davies, suggested that the “emergency is an existential threat to communities everywhere”. Dame Davies was “honoured” to host the event, which “represents a pivotal milestone for the world to move forward together and play a part in safeguarding our antibiotics for generations to come”.
“I call on everyone to join us to make equity, One Health, and action the cornerstone of our next steps to tackle AMR.”
Dr Colin Brown, Deputy Director of Clinical and Emerging Infections at UKHSA, is concerned that “simple lifesaving interventions in the form of antimicrobials are in danger of becoming ineffective”.
“Tackling the issue is a priority for UKHSA but long-term success requires global action. For antimicrobials to remain available and work effectively for everyone, we need international surveillance to identify new areas of AMR and collaboration. We also need to ensure expertise is being shared to help uncover new approaches to therapies and diagnostics for treating drug-resistant diseases.”
WHO’s BPPL
WHO’s updated BPPL “incorporates new evidence and expert insights” to inform R&D for new antibiotics and “promote international coordination to foster innovation”. Dr Yukiko Nakatani, WHO’s Assistant Director-General for Antimicrobial Resistance ad interim, believes the list is “key” to “guiding investment and grappling with the antibiotics pipeline and access crisis”.
“Since the first Bacterial Priority Pathogens List was released in 2017, the threat of antimicrobial resistance has intensified, eroding the efficacy of numerous antibiotics and putting many of the gains of modern medicine at risk.”
Dr Jérôme Salomon, WHO’s Assistant Director-General for Universal Health Coverage, Communicable and Noncommunicable Diseases, stated that AMR “jeopardises our ability to effectively treat high burden infections”, which leads to “severe illness and increased mortality rates”.
The list
Critical priority:
- Acinetobacter baumannii, carbapenem-resistant;
- Enterobacterales, third-generation cephalosporin-resistant; and
- Enterobacterales, carbapenem-resistant;
- Mycobacterium tuberculosis, rifampicin-resistant (included after an independent analysis with parallel tailored criteria, and subsequent application of an adapted multi-criteria decision analysis matrix).
High priority:
- Salmonella Typhi, fluoroquinolone-resistant
- Shigella spp., fluoroquinolone-resistant
- Enterococcus faecium, vancomycin-resistant
- Pseudomonas aeruginosa, carbapenem-resistant
- Non-typhoidal Salmonella, fluoroquinolone-resistant
- Neisseria gonorrhoeae, third-generation cephalosporin- and/or fluoroquinolone-resistant
- Staphylococcus aureus, methicillin-resistant
Medium priority:
- Group A streptococci, macrolide-resistant
- Streptococcus pneumoniae, macrolide-resistant
- Haemophilus influenzae, ampicillin-resistant
- Group B streptococci, penicillin-resistant
AMR returns to the Congress agenda in Barcelona this year, so do get your tickets to be part of essential conversations on how the vaccine community can contribute to the addressing the problem, and don’t forget to subscribe for more insights here.

by Charlotte Kilpatrick | May 8, 2024 | Global Health |
Our next conversation from The World Vaccine Congress in Washington is with Economist Impact‘s Latifat Okara, who joined us to Chair the Market Access track and to discuss the “significance of robust health and economic data in tackling antimicrobial resistance” in the AMR Workshop. Latifat is Principal for Health Policy and Insights, leading up all the team’s research work and insights work for health policy.
Robust data
We first consider Latifat’s session on “robust” data, asking what this means and how it can be achieved. Latifat puts this in the context of AMR.
“What this really means in essence is having thorough and fit-for-purpose data for use as we think about tackling antimicrobial resistance.”
Latifat refers to a report from 2023, which considers an economic model to understand health costs. This research highlighted that, while we have about 16.4 million hospital-acquired infections across 6 emerging economies, there are “still a lot of opportunity gaps”. Furthermore, despite the increasing awareness and attention to antimicrobial resistance, we lack data.
“Without the right data, it’s difficult to measure progress, and without measurement then you really can’t do anything about it.”
Latifat states that, in order to “move the needle”, we need to start thinking about generating “quality data” to use as a “powerful tool” in different conversations.
Why this matters for vaccines
Latifat kindly explains her reasons for emphasising the importance of “robust” data at a vaccine event.
“First of all, without data, there can’t be measurement; without measurement, there can’t be action.”
For the vaccine community, identifying gaps and needs requires data that “cuts across” all levels.
“We need to ask the right questions.”
This goes beyond supplying vaccines to the people who need them; Latifat believes it has economic benefits such as expansion into markets and a “whole lot more”.
Why WVC?
As always, we conclude by asking our experts to share their intentions or expectations for the event, unpacking why they joined us. For Latifat, “practical tools” were key.
“When we think about public health in general, there is a lot of theoretical methods and approaches…but I think for me it’s really important to know how do we take those tools and take it to those who actually need.”
Referring to Dr Cohen’s keynote session, Latifat considers how immunisation can be used at country level.
“How can we actually take the lessons from everything that we’ve learnt from the pandemic…how can we put it to good use?”
In her final comment, Latifat emphasises the importance of breaking the inevitable public health siloes and fostering collaboration.
“I see a lot of organisations here trying to foster that collaboration, which I really commend and encourage.”
It was a pleasure to hear these insights from Latifat, and we hope that you enjoy the interview.
For more conversations with our experts from the Congress in April do make sure you subscribe for weekly updates here!

by Charlotte Kilpatrick | Apr 10, 2024 | Technology |
The Royal Berkshire Foundation Trust announced in April 2024 that initial results from a long-term follow-up study of the safety and effectiveness of an oral spray-based vaccine against urinary tract infections (UTIs) are promising. The study reveals that in both men and women with “recurrent UTIs”, 54% of participants remained UTI-free for up to nine years after the vaccine was administered. Furthermore, they reported no notable side effects.
UTIs
UTIs are described as a “common” bacterial infection, often treated by antibiotics. Around half of women and one in five men experience these “painful and uncomfortable” infections. However, as antibiotic resistant UTIs are “on the rise” and drugs become less effective, there is a need for new ways of preventing and treating the infections.
MV140 in trial
A new solution could be emerging in the form of an oral vaccine: MV140. MV140 is administered through two sprays under the tongue every day for three months. The vaccine was developed by Spain-based pharmaceutical company, Immunotek, and contains four bacterial species in a suspension with water. It has been studied for short-term safety and effectiveness, but this is the first long-term follow-up study. It involved 89 patients who were originally treated privately at The Urology Partnership Reading.
The follow-up study allowed researchers to analyse data from the electronic health records of the original cohort from 2017. They interviewed participants about their experience of UTIs and asked them about side effects. 48 participants remained “entirely infection free” during the nine-year follow-up. The average infection-free period across the cohort was 54.7 months (four and a half years). 40% of participants reported having repeat doses of the vaccine after one or two years.
Safe and effective
Dr Bob Yang is a Consultant Urologist at the Royal Berkshire NHS Foundation Trust and co-led the research, commenting that prior to taking the vaccine “all our participants suffered with recurrent UTIs, and for many women, these can be difficult to treat”.
“Nine years after first receiving this new UTI vaccine, around half of participants remained infection free. Overall, this vaccine is safe in the long term and our participants reported having fewer UTIs that were less severe.”
Indeed, if participants did report UTIs, they were able to treat these infections by “simply drinking plenty of water”. Not only is the vaccine effective, but it is “a very easy vaccine to administer” and “could be given by GPs as a 3-month course”.
“Many of our participants told us that having the vaccine restored their quality of life. While we’re yet to look at the effect of this vaccine in different patient groups, these follow-up data suggest it could be a game changer for UTI prevention if it’s offered widely, reducing the need for antibiotic treatments.”
Professor of Urology at the Alta Uro Medical Centre for Urology in Switzerland, and EAU Chair of Guidelines on Urological Infections, Gernot Bonkat, thinks the “findings are promising”.
“Recurrent UTIs are a substantial economic burden and the overuse of antibiotic treatments can lead to antibiotic-resistant infections.”
Although Professor Bonkat highlights the need for “further research”, the study “reveals encouraging data”.
“While we need to be pragmatic, this vaccine is a potential breakthrough in preventing UTIs and could offer a safe and effective alternative to conventional treatments.”
Could this vaccine offer hope to the many people who experience UTIs and contribute to the fight against AMR? For more like this, don’t forget to subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Apr 9, 2024 | Global Health |
In an article for npj vaccines, a group of experts present an approach to effectively and efficiently evaluate vaccines against antimicrobial-resistant (AMR) pathogens. The approach, which they call Reverse Vaccine Development, evaluates proof-of-principle efficacy “as early as possible” in a population with a high incidence of disease. The authors suggest that their method “may be the only way” to deliver life-saving vaccines to populations affected by AMR-pathogen diseases at incidences that are “typically low and unsuited” to Phase III efficacy trials. Here, we examine the proposal and invite you to share your reactions to it.
The burden of AMR and the need for vaccines
The paper states that a “recent estimation” of the burden of AMR on global human health indicates a “medical need comparable and likely larger than HIV and malaria”. In response, the vaccine community is targeting AMR pathogens. However, the development of these vaccines is “being hindered” by a “lack of understanding of their correlates of protection”.
“Vaccine development can be long, difficult, and costly. However, it becomes easier when a correlate of protection is known.”
The recent example of SARS-CoV-2 vaccine development speed is attributed by the authors not only to the “extraordinary” efforts of companies and authorities, but also to the knowledge of the “likely mechanism of protection”: “antibody to the spike protein preventing interaction with the host cell”. In contrast, for many of the human pathogens, including WHO’s list of global priority pathogens of antibiotic-resistant bacteria, the mechanism of protection “remains unknown”.
“Without a correlate of protection, late-stage clinical development is risky: many thousands of research participants may be needed for efficacy evaluations, and after many years of R&D and large expense, the trials may fail.”
Reverse Vaccine Development
The paper claims that, whilst developing a vaccine candidate against S. aureus, they identified a need for a “new vaccine development paradigm”, wherein data generation on efficacy and immune responses “should occur early”, instead of in Phase III. This starts with a Phase I/II study to assess safety, immunogenicity, and efficacy. If the vaccine is First-Time-in-Human (FTiH), a Phase I safety lead-in study could be needed to escalate dose. If there are no safety issues, the Phase II can “proceed to evaluate immunogenicity and efficacy”.
An important note is raised: the population used for the efficacy assessment must have a “high attack rate”. However, the attack rate may not be high in the population intended for registration. Thus, Reverse Vaccine Development “requires a population with a high attack rate” that is “available for study”. For example, the authors’ S. aureus vaccine candidate has such an available population: patients with a community acquired skin and soft tissue infection, for whom risk of recurrence is high.
“An efficacy evaluation of a candidate vaccine early in clinical development is of key importance. If the vaccine is found not efficacious, unnecessary exposure of subjects to the vaccine is avoided. If the vaccine is efficacious, correlates of protection can be explored.”
The success of Reverse Vaccine Development “depends on the number and validity” of the immunological readouts, and antibody titers in isolation are “likely insufficient”. The following “immunological parameters” are suggested:
- Systems serology – offers unbiased and comprehensive data for identifying previously unappreciated processes and mechanisms.
- Cellular responses – should be evaluated to understand the flavour of the induced T-cell response or if the vaccine increases the frequency of T cells specific for the vaccine antigens.
- Transcriptional profiling – provides a complementary and broad view of the immune response to a vaccine.
- Assessment of multiple immunological signals that correlate with each other – can increase the chance of identifying a signature of protection.
- Assessment of memory responses.
- Assessment of background immunity.
The authors suggest that Reverse Vaccine Development is “most suited” to the development of vaccines against pathogens for which a correlate of protection is not known, which hinders preclinical and/or clinical development.
What does this mean for the community?
The perspective concludes that the authors’ approach “assesses vaccine efficacy in the early phases” of development with the potential to identify a correlate of protection.
“Reverse Vaccine Development has the potential to facilitate the development of vaccines against AMR pathogens.”
How might this approach support your work or facilitate faster or more effective vaccine development? Vaccines for AMR pathogens were a key concern that arose at the Congress in Washington this April, so we expect to continue exploring this subject throughout the year with expert insights from our community. Don’t forget to subscribe to get these delivered to your inbox weekly.

by Charlotte Kilpatrick | Mar 13, 2024 | Global Health |
In March 2024 Pfizer announced that the European Commission (EC) has granted marketing authorisation for the company’s 20-valent pneumococcal conjugate vaccine, which is marketed in the EU as PREVENAR 20, for active immunisation for the prevention of invasive disease, pneumonia, and acute otitis media caused by Streptococcus pneumoniae in infants, children, and adolescents between the ages of 6 weeks and 18 years.
The authorisation is valid in the 27 EU Member States along with Iceland, Lichtenstein, and Norway. This announcement comes shortly after a positive opinion from the European Medicines Agency (EMA)’s Committee for Medicinal Products for Human Use (CHMP) and is almost a year after the approval of PREVENAR 20 for children and infants by the US FDA in April 2023. Further approvals have been granted in countries such as Canada, Australia, and Brazil.
PREVENAR 20
PREVENAR 20 includes 13 serotypes from PREVENAR 13 with seven new serotypes, all of which are “global causes of invasive pneumococcal disease” (IPD). They are associated with “high case-fatality rates, antibiotic resistance, and/or meningitis”. The 20 serotypes contained within the vaccine are responsible for “the majority” of currently circulating pneumococcal disease both in the EU and globally.
Pfizer states that the EC authorisation has been informed by evidence from the Phase III clinical trial programme that comprises four core paediatric studies, which collectively enrolled more than 4,700 infants and 800 toddlers and children of all ages.
A significant opportunity
Alexandre de Germay is Pfizer’s Chief International Commercial Officer and Executive Vice President and described the authorisation as a “significant opportunity to improve public health”.
“PREVENAR 20 builds on Pfizer’s decades-long commitment to develop vaccines to help prevent potentially life-threatening infections, and we are proud to now provide the broadest serotype coverage of any pneumococcal conjugate vaccine for children in Europe.”
Pfizer’s Dr Kara Bickham will participate in a panel on the future of novel pneumococcal vaccines at the Congress in Washington this April, so do join us for this to learn more about Pfizer’s programme and ambitions, and don’t forget to subscribe to our newsletters here.

by Charlotte Kilpatrick | Feb 29, 2024 | Infection |
In February 2024 Mass Eye and Ear announced the publication of a paper in Proceedings of the National Academy of Sciences (PNAS) that describes the discovery of 18 “never-before seen species of bacteria of the Enterococcus type” in research to understand antibiotic resistance. Antibiotic resistance (AMR) is a growing global health threat, with antibiotic-resistant infection “projected to catch up to cancer” as the leading cause of death by 2050.
Introducing Enterococci
The paper describes enterococci as “unusually rugged and environmentally persistent microbes”. Their “unusual hardiness” is understood to contribute to the spread of antibiotic-resistant enterococci in hospitals. They are “among the most widely distributed members of gut microbiomes in land animals”. However, their occurrence varies “widely”, which offers a “unique opportunity to explore how diverse host backgrounds” drive microbiome membership.
The study
The authors intended to “sample the Earth broadly” for “enterococci from diverse hosts, geographies, and environments”. This would offer a “first approximation of the diversity of species on the planet” and allow comparison of the “content and degree of divergence of their genomes toward the broader goal of understanding the mechanisms that drive association with particular hosts”.
To do this, they collected and taxonomically identified at DNA sequence level 430 enterococci from unprocessed animal samples and 456 enterococci isolated by contributors from diverse sources; the result was a collection of 886 isolates. Then they sequenced the entire genomes of strains that exhibited sequence diversity “suggestive of distant relationship to any known species”, which identified 18 “previously undescribed species” of Enterococcus and 1 new species of the ancestrally related genus Vagococcus.
Relevance for AMR infections
The paper emphasises that developing an understanding of “host association principles” is “imperative”. By isolating 18 “previously undescribed species” they determine that “much species-level diversity” within the genus “remains to be discovered”. Dr Michael S. Gilmore, director of the Infectious Disease Institute at Harvard Medical School and Chief Scientific Officer at Mass Eye and Ear, recognised that “over the past 75 years” antibiotics have “saved hundreds of millions of lives” and “contributed greatly to the success of all types of surgery”.
“Over the past 30 years, however, many of the most problematic bacteria have become increasingly resistant to antibiotics and this is now reaching crisis proportions. Our findings may improve understanding of how resistance genes spread to hospital bacteria and threaten human health.”
Dr Gilmore suggests that insects have been eating rotting plant material, where antibiotics are naturally produced by microbes in the soil. They have therefore been dosing themselves with antibiotics, exposing the bacteria in their gut to these antibiotics and encouraging resistance.
“The COVID-19 pandemic revealed that nature contains many infectious risks for humans. This study shows that insects and their relatives in nature are a large and uncharacterised reservoir of undiscovered genes in microbes closely related to those that cause some of the most antibiotic resistant infections.”
Dr Ahslee Earl, director of the Bacterial Genomics Group at Broad, commented that, “until recently, most of what we’ve understood about the genetics of enterococcus come from those that make us sick”. However, this is a “problem” that is “like trying to understand darkness without ever seeing the light”.
“Expanding our view to include those from outside of hospitals, with the help of citizen scientists, gave us the contrast we needed to identify how they make people sick in the hospital, and also gives the public the chance to co-own solutions.”
AMR is a key workshop theme at the Congress in Washington this April, so do join us to participate in the discussions about how vaccines can contribute to managing the problem. For more research insights, why not subscribe to our newsletters here?

by Charlotte Kilpatrick | Feb 23, 2024 | Global Health |
In February 2024 SK bioscience announced that the company had been granted prequalification (PQ) certification from WHO for SKYTyphoid, its typhoid conjugate vaccine. Jointly developed with IVI and supported by the Bill & Melinda Gates Foundation, the vaccine uses the “purified Vi polysaccharide-diphtheria conjugate” method. It can be administered to infants and children between the ages of 6 months and 2 years. There are between 11 million and 20 million typhoid fever cases reported globally each year, resulting in around 120,000 to 160,000 deaths.
SKYTyphoid
The purified Vi polysaccharide-diphtheria conjugate method conjugates a polysaccharide of typhoid bacteria, serving as an antigen, to a diphtheria toxin protein, which serves as a carrier. This vaccine is expected to offer “comparable immunogenicity” and “long-term protection” through a single dose in comparison with existing oral live or polysaccharide typhoid vaccines.
WHO’s PQ ensures that the vaccine has complied with “stringent” procedures and protocols. SK bioscience states that the vaccine has already received an export license from the Korean Ministry of Food and Drug Safety thanks to the results of a Phase III study in Nepal. Now, with WHO’s seal of approval, SK bioscience “plans to target global markets”, focusing on public procurement markets, including major typhoid-endemic countries with “high demands”.
Vaccination critical to prevention
Jaeyong Ahn is SK bioscience’s CEO and is “pleased” that the “global collaboration to address the global vaccine supply imbalance and improve public health” has been “recognised” by this certification.
“We will make every effort to rapidly supply SKYTyphoid by obtaining approvals in countries.”
Dr Jerome Kim, Director General of IVI, reflected that “Typhoid fever is more prevalent in warmer temperatures”. Therefore, “climate change and the worrying rise of antimicrobial resistance are only adding to the threat” posed by the disease.
“Vaccination is critical to effective prevention and control of the disease. In collaboration with SK bioscience and other partners, IVI will continue endeavours to make this vaccine accessible to people who need it the most.”
We look forward to hearing more from Dr Kim and representatives from SK bioscience at the Congress in Washington this April. To join us there get your tickets today, and don’t forget to subscribe for more insights!

by Charlotte Kilpatrick | Feb 23, 2024 | Technology |
In February 2024 LimmaTech Biologics announced positive interim data from a Phase I/II trial evaluating Shigella4V (S4V). S4V is a tetravalent bioconjugate vaccine candidate against shigellosis, an infectious disease that is cause by Shigella bacteria. Shigellosis is the second leading cause of fatal diarrhoeal disease and is most dangerous in infants in low- and middle-income countries. The vaccine candidate has been in-licensed from GSK to advance clinical development.
LimmaTech states that an estiamted 188 million infections are due to Shigella, of which 62.3 million are in children under five. ALthough the standard treatment is oral rehydration and antibiotic therapy, the bacteria have acquired resistance to many antibiotics and there is no licensed vaccine.
S4V in trial
The vaccine candidate is a tetravalent bioconjugate vaccine that encompasses the O-antigen polysaccharides of S. flexneri 2a, 3a, 6, and S. sonnei. It targets that four predominant pathogenic Shigella serotypes responsible for “up to 85%” of global infections.
The Phase I/II study is conducted in Kenya; it is a randomised, double-blind, dose-finding, age-descending clinical trial to assess the safety and immunogenicity of S4V. The trial is divided into two elements, the first of which evaluated the vaccine candidate’s safety in adults, children (aged 2-5), and infants. The second part evaluated S4V’s safety and immunogenicity in the nine-month-old target population to determine the preferred dose.
Positive results
The latest data from the second part of the trial includes 472 infants who received two intramuscular injections at one of four dose levels, with or without an adjuvant. S4V was “well tolerated” with most reactions being “mild” and “similarly distributed” over the different groups. No vaccine-related serious adverse events (SAEs) were reported.
Dr Patricia Martin, Chief Operating Officer at LimmaTech, commented that the “positive interim results” demonstrate “very good immunogenicity” in infants, the “population that needs it the most”.
“Shigellosis is a serious disease caused by a pathogen continuously evolving and becoming increasingly resistant to antibiotics. Our vaccine candidate has the potential to prevent an infection that threatens the lives of many children.”
Furthermore, the candidate could have uses for “travellers and military personnel”. Dr Martin is excited for the continued clinical development of the vaccine.
To participate in discussions about the role that vaccines can play in tackling the issue of antimicrobial resistance do join us in Washington this April for the Congress or subscribe to our newsletters here.