by Charlotte Kilpatrick | Oct 24, 2024 | Technology |
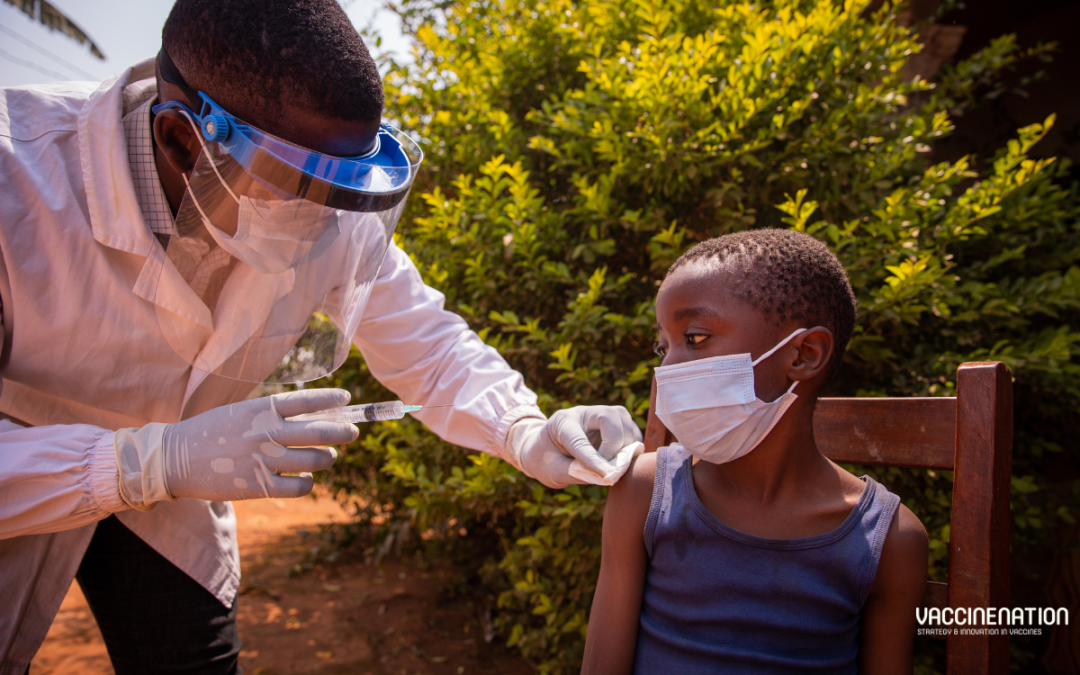
The University of Connecticut (UConn) announced in October 2024 that associate Professor Thanh Nguyen’s research has received “significant” backing from The Bill and Melinda Gates Foundation. The Gates Foundation has awarded a series of grants totalling $6.6 million, following support from the National Institutes of Health (NIH) and the US Department of Agriculture (USDA). The funding will contribute to research and innovation for a microneedle array patch that can deliver multiple human vaccines at once. The Foundation initially awarded $2 million, which has increased after early success.
Microneedle array patch technology
Dr Thanh Nguyen works in the College of Engineering’s School of Mechanical, Aerospace, and Manufacturing Engineering. His microneedle method is “far less painful” than traditional syringe delivery and offers access and uptake benefits.
“What if we were able to mail people vaccines that don’t need refrigeration, and they could apply to their own skin like a bandage?”
The technology delivers highly concentrated vaccines in powder from over months, through a “nearly painless” 1-centimetre-square biodegradable patch.
“The primary argument is that getting vaccines and boosters is a pain. You have to go back two or three times to get these shots. With the microneedle platform, you put it on once, and it’s done.”
Funding increases
After the initial award of $2 million, the project made good progress and received additional funding to support the development of a scale-up manufacturing technology to produce patches on an industrial scale. In late September, the Gates Foundation awarded $4 million to take the patch “a step farther” as a pentavalent and Polio vaccine targeting diphtheria, tetanus, pertussis, HIV, Hepatitis B, and Polio. With this funding, the team can “build up productivity”. They are partnering with LTS to scale up production and are expanding the size of laboratory.
The award also marks a fundraising milestone for Dr Nguyen, who has earned more than $25 million in research awards, which he reflects “doesn’t come naturally”.
“It comes from the recognition of the high impact of the research and the lab’s success in publishing articles. It is a testament to the importance of what we are doing.”
For the latest vaccine development and technology updates, don’t forget to subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Oct 23, 2024 | Global Health |
A study in The Lancet Global Health sought to provide counterfactual scenarios to evaluate the short-term effects of different vaccination strategies on mpox cases and deaths in the Democratic Republic of the Congo (DRC). The researchers used a dynamic transmission model to simulate mpox transmission, stratified by age and province; this was used to assess potential vaccination strategies and their effects on deaths and cases in an epidemic year. The results indicate that vaccinating children aged 15 years or younger, or younger than 5 years, in endemic regions, would be the “most efficient use of vaccines” when resources are limited.
Mpox in DRC
Mpox was first identified in the Democratic Republic of the Congo (DRC) in 1970; it is a zoonotic infectious disease caused by the monkeypox virus (MPXV), which is endemic in “numerous regions” of west and central Africa. MPXV has two clades:
- Clade I is endemic in central Africa with an estimated case fatality rate of up to 10% and mainly affecting children. It is divided into two subclades, Ia and Ib.
- Clade II was historically found in west Africa, with an estimated case fatality rate of up to 1%-3%. It is also divided into two subclades, IIa and IIb. Clade IIb was responsible for the global mpox epidemic in 2022.
The authors state that, until 2022, MPXV was not associated with large outbreaks; most cases were related directly to sylvatic transmission from animals to humans via hunting, wild game preparation, and consumption. Increases in human-to-human transmission were identified in 2017.
The researchers suggest that the low likelihood of transmission in the early decades after the virus’ discovery could be related to smallpox eradication programmes, which offered cross-immunity via vaccination against a related orthopoxvirus. Indeed, since the cessation of the smallpox vaccination programme in the DRC, there has been a “concurrent increase in mpox cases and outbreak frequency”. There is an ongoing, “unprecedentedly large” outbreak of clade I mpox in the DRC, with more than 14,000 reported suspected cases by the end of 2023 and a 4.6% case fatality rate. Over 70% of the deaths are in children younger than 15 years.
Genetic analyses of clade Ia MPXV genomes indicate that in this outbreak, multiple, independent zoonotic introductions into the human population have occurred from one or more reservoir species. An increasing burden of clade Ib MPXV infections have been identified in eastern DRC with evidence of “sustained” human-to-human transmission and many cases in women aged 15-29 years, but clade Ia infections continue to comprise most mpox cases in the DRC.
The study
Bavarian Nordic’s modified vaccinia Ankara vaccine (JYNNEOS) is protective against mpox. It was approved by the US FDA in 2019 but was not widely used against mpox until the 2022 outbreak, when it was “quickly mobilised to vaccinate people at high risk of infection in the USA and Europe”. Despite its high efficacy at two doses, it is “largely unavailable” outside the USA and Europe.
The authors aimed to inform policy and decision makers on the “potential benefits of, and resources needed,” for mpox vaccination campaigns in the DRC. They used an approach based on models from operations research and decision science to offer a robust analysis of policy choices “even in the context of incomplete and uncertain data”. The study uses mathematical modelling to simulate the spread of mpox in the DRC during 2023.
Without vaccination, the model predicted 14,700 cases of mpox and 700 deaths from mpox in the DRC over 365 days, consistent with reported estimates. Almost 50% of the cases and deaths came from the province of Equateur. Cases were evenly split between the three age groups: 34% in children under 5 years, 32% in children aged 5-15 years, and 34% in people older than 15 years. However, deaths were “predominantly” seen in children younger than 5 years (51%).
Vaccinating 80% of children younger than 5 years in all provinces or provinces with a history of mpox cases decreased the outbreak to 10,500 cases and 400 deaths. Vaccinating in endemic provinces increased cases to 10,700 and deaths remained the same. The numbers of vaccine doses needed for the strategies were 41.4 million (all provinces), 33.8 million (provinces with a history of mpox), and 13.2 million (endemic provinces only).
Vaccinating 80% of children younger than 15 years in all provinces or provinces with a history of mpox cases decreased the outbreak to 6,400 cases and 200 deaths. Vaccinating in endemic provinces increased cases to 6,800 and deaths remained the same. The numbers of vaccine doses required for these strategies were 81.6 million (all provinces), 67.1 million (provinces with a history of mpox), and 26.6 million (endemic provinces only).
Vaccinating 80% of all ages in all provinces or only non-endemic provinces with a history of cases decreased the case burden to 1,400 cases and 100 deaths, and 2,000 cases and 100 deaths when vaccinating in provinces endemic for mpox. The numbers of doses required for these strategies were 170.8 million (all provinces), 142.0 million (provinces with a history of mpox), and 56.8 million (endemic provinces only).
Managing resources
The paper finds that vaccinating all ages leads to the “largest impact on magnitude of cases and deaths”, but that vaccinating only children aged 15 years or younger provides “nearly the same effect with fewer vaccine doses required”. Although vaccinating only children younger than 5 years showed a “drop-off” in averted cases and deaths, it provides the most efficiency.
“This analysis shows the effectiveness of focussing an mpox vaccination campaign specifically in the provinces endemic for mpox in the DRC. This targeted strategy prevents nearly as many cases and deaths as broader approaches but uses fewer vaccine doses and thus would be less costly to implement.”
Alexandra Savinkina, fourth year PhD student in the Yale School of Public Health (YSPH) Department of Epidemiology (Microbial Diseases), commented that this study could influence vaccination policy.
“My hope is that it could help inform policy for vaccination in the country and potentially the region and move the needle forward on getting vaccines to the people who need them most in the DRC.”
Savinkina hopes that “we can learn from the global mpox outbreak that we can’t ignore disease in other places”.
“If the resources to help people exist, I think we should be using them, whether in the U.S. or in Africa.”
Dr Gregg Gonsalves, associate professor of epidemiology at YSPH, acknowledged barriers to access.
“We take it for granted that we can get a vaccination for COVID or a flu shot at our local CVS, but the infrastructure to deliver vaccines in DRC is far less robust.”
For more vaccine research updates, subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Oct 18, 2024 | Technology |
In October 2024 the Animal and Plant Health Agency (APHA) and The Vaccine Group (TVG) announced that Innovate UK has awarded them a Smart grant in excess of £400,000 to advance a novel viral vector platform. In a project lasting 19 months, the two organisations will use technology developed by TVG scientists in candidate vaccines for two “important diseases in cattle”: bovine respiratory syncytial virus (BRSV) and lumpy skin disease (LSD). The project will continue previous research, which identified potential vaccine candidates; it is supported by the World Reference Laboratory for Non-Vesicular Diseases at The Pirbright Institute, determining how the candidates can produce an adequate serological response in animals and protect cattle.
BRSV and LSD
Bovine respiratory syncytial virus (BRSV) is the leading viral cause of respiratory illness in young calves in the UK. It affects around 1.9 million calves each year, costing approximately £54 million. It is “prevalent worldwide” and poses a “substantial economic burden” on beef and dairy producers. In the past 10 years, lumpy skin disease (LSD) has spread “dramatically” beyond former natural enzootic geographies in Africa and the Middle East to cause “severe disease” in other regions.
Both diseases have “broad global prevalence”, and BRSV particularly affects intensively reared cattle. Currently available commercial vaccines for BRSV do not prevent shedding and are restricted from use in young calves by maternal immunity. There are no DIVA (differentiating infected from vaccinated animals) vaccines available for LSD, so use is limited to areas where serosurveillance and eradication programmes are in place.
TVG’s vaccine solutions
The Vaccine Group (TVG) hope to address these challenges. With “key opinion leaders” for the two diseases in the UK and Canada, TVG has inserted transgenes for protective antigens from each virus into two separate constructs through genetic manipulation. Both vaccine candidates have been shown to be genetically stable and have demonstrated “stable and prolonged” protein expression in tissue culture over multiple passages. The technology works by introducing a benign virus to cattle, which stimulates the expression of proteins to induce an immune response.
Chief Executive Officer at TVG, Dr Jeremy Salt, reflected that infectious diseases are a “major cause for concern” for cattle farmers around the world, leading to “significant losses – both in terms of animal health and welfare, and in financial terms”.
“Our goal in developing a viral vector platform for use in cattle effective vaccines is to overcome some of the deficiencies that affect the current commercialised vaccines. By doing so, we can better protect the farmers, their animals, and their livelihoods.”
Dr Salt also hopes to “make beef and milk production more efficient, humane, and sustainable”, whilst “helping the sector address the global challenges of antibiotic resistance and carbon emissions”.
We look forward to hearing from Dr Salt at the Congress in Barcelona in just a few weeks; get your tickets to join us there and don’t forget to subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Oct 17, 2024 | Global Health |
A study in The Lancet Global Health estimates the impact that the 100 Days Mission could have had on the COVID-19 pandemic. The authors find that the implementation of non-pharmaceutical interventions (NPIs) within the 100 Days Mission could have averted around 8.33 million deaths, corresponding to a monetary saving of US$14.35 trillion. Investment in manufacturing and health systems contribute an increase to 11.01 million deaths averted. The researchers comment on the value of the 100 Days Mission but emphasise the importance of “prioritising a more equitable global vaccine distribution”.
In search of greater vaccine benefits
Although COVID-19 vaccines are estimated to have prevented almost 20 million deaths, the authors demand a better understanding of the “further health and economic benefits that could have been achieved” through shorter development times and “improved global equity in pandemic preparedness”. CEPI’s 100 Days Mission was proposed in 2021, establishing the ambition of cutting vaccine development time for new pathogens to 100 days. This about a third of the time taken to deliver the first COVID-19 vaccine.
“The availability of COVID-19 vaccines within 100 days would have substantially changed the pandemic; however, these benefits would be finite without enabling equitable access to vaccine products through system equity.”
Various efforts to encourage global vaccine distribution were “hampered” by inequities, and it is recognised that manufacturing capacity should be “expanded but also diversified” to “promote self-sufficiency and regional resilience”. Furthermore, supply chains and infrastructure must be scaled to enable the delivery of vaccines that rely on cold-chain infrastructure.
The study
The searchers hoped to quantify the potential impact of the 100 Days Mission by retrospectively estimating the effect it would have had on the COVID-19 pandemic, thus offering evidence to support decision making around future investments in research and development capabilities. They also aimed to quantify the impact of “additional investments”.
The analyses use an extended version of a previously published compartmental susceptible-exposed-infectious-recovered transmission model of COVID-19 vaccination with an explicit healthcare pathway. The vaccination pathway was expanded to include booster vaccination alongside waning efficacy, capturing the “restoration of immunity” through booster doses. The new vaccination pathway was parameterised to match platform-specific vaccine efficacy data and the duration of protection.
The authors modelled the impact of the 100 Days Mission by simulating a counterfactual scenario where the global vaccination campaign began on 20th April 2020, 100 days after the publication of the full SARS-CoV-2 genome. This scenario assumes that vaccinations in each country took the same roll-out process, but 232 days earlier. Two additional scenarios reflected “increased investment” in research and delivery infrastructure.
The Manufacturing scenario removed supply constraints, enabling the rollout of vaccination on 20th April 2020 in every country, without stockouts. The infrastructure-equity scenario enhanced both national health systems and global distribution networks so that all countries achieved 40% vaccine coverage in the first year and 40% booster coverage in the second year.
To account for the relaxing of non-pharmaceutical interventions (NPIs), the authors simulated three scenarios for NPI relaxation speeds as vaccination coverage improved. The History scenario assumed no changes, whereas the Target and Economic scenarios assumed earlier relaxing; the Target scenario lifted all restrictions over two months after reaching more than 80% adult coverage in high-income countries or more than 80% coverage in those older than 60 in other countries. The Economic scenario lifted NPIs more gradually after reaching the over-60 target, prioritising the reopening of schools.
Study findings
The results suggest that the 100 Days Mission could have averted an additional 8.33 million deaths due to COVID-19 by the end of 2021 when combined with the History NPI lifting scenario. In this scenario, an estimated 26.72 million severe cases of COVID-19 requiring hospitalisation and 1/44 billion infections would have been averted. Most of these averted deaths, hospitalisations, and infections would have occurred in low- and middle-income countries (LMICs).
The estimated VSLs (value of a statistical life) that could have been saved by the 100 Days Mission through the History scenario is US$22.61 trillion globally. As VSLs are “significantly higher” in HICs, 57% of the global value of statistical life averted occurred in HICs, even though most deaths would have been averted in LMICs. To estimate the monetary values associated with lives saved the authors multiplied the number of lives saved by the country-specific monetary VSL and by the value of a statistical life-year (VSLY).
“Increased investment in both global manufacturing and health systems infrastructure further increases the number of deaths that could be averted and the associated health-economic savings.”
In the 100 Days Mission with both manufacturing and health systems investments, an estimated 11.01 million deaths could have been averted and a value of $31.29 trillion in statistical lives saved. However, the authors describe this scenario as “unlikely”. In all scenarios involving the relaxing of NPIs thanks to earlier availability of vaccines, additional lives would have been saved.
In the Target NPI lifting scenario, an estimated 5.76 million deaths (100 Days Mission alone) to 9.20 million deaths (100 Days Mission with both manufacturing and infrastructure investments) could have been averted. In these scenarios, 12,600 and 23,900 fewer days of NPIs would have been implemented globally: 70 days and 133 days on average per country. Under the Economic scenario there were “similar trade-offs between public health and economic gains”. The public health and health economic outcomes would be greater than under the Target scenario, but still lower than the History scenarios.
Substantial benefits
“Earlier access to COVID-19 vaccines could have had substantial benefits.”
Most of the estimated averted deaths would have been concentrated in LMICs, but this demands investments in vaccine research, supported by “improvements to manufacturing and health system infrastructures”. With these investments, the authors estimate that 11 million deaths could have been prevented globally.
Although NPIs were effective at reducing transmission they incurred “significant economic and societal costs”, including consequences for education. Therefore, a major benefit of earlier access to vaccination is the reduction in school closures; in the Economic scenario, prioritising school opening could have averted 1,120 weeks of full school closures and 2,490 of partial school closures. This represents an average of 6 weeks of fully open schools and 14 weeks of partly open schools per country.
“Reopening schools and relaxing NPIs safely will crucially require scaling up both vaccine delivery infrastructure and manufacturing. Without addressing both aspects, advancements in vaccine development speed might not translate into equitable benefits globally.”
The results emphasise the importance of investments in support of the 100 Days Mission in controlling a future potential pandemic, with benefits for both health and economy.
“The 100 Days Mission is ambitious, requiring global innovation through creating vaccine libraries, clinical trial networks, accelerated immune response marker identification, rapid vaccine manufacturing, and strengthened global disease surveillance.”
CEO of CEPI, Dr Richard Hatchett, hopes that this research will encourage global commitment to the 100 Days Mission.
“This work shows in the starkest terms why the world needs to be prepared to move faster and more equitably when novel pandemic disease threats emerge. Investing in preparedness now to make the 100 Days Mission possible for future incipient pandemics will save millions upon millions of lives and protect the global economy against catastrophic losses.”
Join us at the Congress in Barcelona this month to explore how lessons from the COVID-19 pandemic can inform better global preparedness for pandemic and epidemic pressures, and don’t forget to subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Oct 16, 2024 | Technology |
A paper in Nature Biotechnology in October 2024 presents an “end-to-end clinical proteogenomic pipeline” to address the challenges associated with identification and prioritisation of antigenic peptides. NeoDisc combines “state-of-the-art publicly available and in-house software” with in silico tools to identify, predict, and prioritise tumour-specific and immunogenic antigens from multiple sources. The authors demonstrate the pipeline’s superiority over recent prioritisation pipelines and showcase the features that enable “both rule-based and machine-learning approaches”. They also reveal how NeoDisc’s multiomics integration identifies “defects in the cellular antigen presentation machinery”.
Antigen discovery
The researchers comment on the importance of personalised antigen discovery for the development of cancer vaccines. Common approaches for translational research and clinical trials include whole-genome sequencing (WGS) or whole-exome sequencing (WED) and RNA sequencing (RNAseq). However, the recent application of mass spectrometry (MS) to identify HLA-bound peptides and the use of proteogenomics have “facilitated the exploration of novel targets from a variety of antigens naturally processed and presented in cancer”.
“Their identification is laborious and current clinical pipelines do not support immunopeptidomics and are restricted to predicted neoantigens.”
Although immunotherapies are “remarkably effective” against some indications, “robust immune pressure” can force immune editing. Therefore, it is “essential” to understand the heterogenous antigenic landscape and the tumour’s capacity to present antigens.
The study
In the study, the authors introduce an “end-to-end” clinical antigen discovery proteogenomic pipeline: NeoDisc. It compiles publicly available and in-house software for the identification of immunogenic tumour-specific HLA-I and HLA-II antigens from genomics and transcriptomics and MS-based immunopeptidomics and enables their prediction and prioritisation with rule-based and machine-learning (ML) tools. It allows assessment of tumour heterogeneity and the functionality of the antigen processing and presentation machinery (APPM). The study compares NeoDisc’s performance with other tools, demonstrating its application for personalised antigen discovery and clinical implementation.
NeoDisc is a “dedicated computational framework” combining genomic, transcriptomic, and immunopeptidomic data and integrating curated public databases of known immunogenic TSAs, TAAs, oncoviral elements, and noncanonical transcripts. It uses matched tumour and germline genomic data for sample-specific variant characterisation, tumour content estimation, and copy number variation (CNV) and somatic mutation (SM) identification.
Four variant-calling algorithms are applied to WES and WGS data; variants that are detected by two or more callers are considered to have “high identification confidence”. Although highly mutated tumours usually respond better to immunotherapy, the selection of immunogenic neoantigens among “numerous possibilities” is “challenging”. Recent screening of large datasets of neoantigens in tumours from 112 participants has allowed the training of ML for prioritisation. ML classifiers trained on a fraction of this dataset have been integrated into NeoDisc to ensure “effective prioritisation”.
When NeoDisc’s rule-based and ML ranking approaches were compared with existing tools, the ML prioritisation algorithm “surpassed all the evaluated tools”. The researchers demonstrated NeoDisc’s “efficient prioritisation” on a cervical adenocarcinoma (CESC-1) characterised by an “exceptionally high mutational burden” (25 SMs per Mb).
Of the 393 identified actionable mutations, representing a pool of 19,051 peptides with a predicted binding rank ≤2%, 66 HLA-I neoantigenic short peptides (minimal epitopes) were selected through rule-based prioritisation for T cell screening of autologous tumour-infiltrating lymphocytes (TILs) by IFNγ ELISpot. 11 of the 66 peptides were immunogenic, including two that “ranked among the top ten candidates”. The NeoDisc ML model reordered the tested neoantigens, resulting in an “impressive” ranking of six immunogenic peptides in the top ten. NeoDisc also successfully identified two confirmed immunogenic neoantigens in the CESC-1 tumour MS immunopeptidomic data.
Personalised vaccines
While the default NeoDisc settings “exhibit good performance”, biopsies with low tumour content and low mutation burden could result in the detection of an “insufficient number of actionable high-confidence expressed mutations”. This would lead to a “suboptimal vaccine”. Thus, NeoDisc offers two additional modes:
- “Sensitive mode” considers the union of mutations called by all four variant-calling tools, to be used when an insufficient number of mutations are detected.
- “Panel mode” uses mutations listed in the available diagnostic clinical gene panel (GP) as input, allowing the design of vaccines for persons lacking dedicated biopsies. Note that GPs “often provide insufficient number of mutations leading to suboptimal lists of neoantigens or potentially none”.
The paper states that, in cancer vaccines, long sequences are favoured over minimal short peptides, motivated by the “efficient uptake and processing by APCs”. The NeoDisc ML tool ranks mutations according to their potential immunogenicity. Long sequences are “optimally” designed through maximised coverage of high-quality predicted HLA-I and HLA-II neoantigens.
In use in the field
NeoDisc is already being used in Phase I clinical trials for personalised cancer vaccines and adoptive T cell therapies in Switzerland; the authors hope that these demonstrate its “practical utility and potential for clinical translation”. Dr Michal Bassani-Sternberg of the Lausanne Branch of the Ludwig Institute for Cancer Research comments that NeoDisc provides “invaluable” insights into the immunobiology of tumours and the “mechanisms by which they evade targeting by cytotoxic T cells”.
“Notably, NeoDisc can also detect potential defects in the machinery of antigen presentation, alerting vaccine designers and clinicians to a key mechanism of immune evasion in tumours that can compromise the efficacy of immunotherapy. This can help them select patients for clinical studies who are likely to benefit from personalised immunotherapy, a capability that is also of great importance to optimising patient care.”
Florian Huber, first author, also reflected on the significance of this research.
“NeoDisc can detect all these distinct types of tumour-specific antigens along with neoantigens, apply machine learning and rule-based algorithms to prioritise those most likely to elicit a T cell response, and then use that information to design a personalised cancer vaccine for the relevant patient.”
Join us at the Congress in Barcelona this month to hear from experts in the Cancer and Therapeutic Vaccines track on their approaches to personalised vaccine development, and don’t forget to subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Oct 15, 2024 | Technology |
In October 2024, Panthera Biopartners announced that Parexel has confirmed its inclusion in the Parexel Site Alliance Vaccine Network. Panthera becomes the first UK public or commercial clinical trial organisation to join the global network of high performing clinical trial sites. Parexel’s Site Alliance Vaccine Network “fosters long-term collaborative relationships” with research organisations across the globe to “deliver efficiencies”. Panthera was chosen to join the Network because of “exceptional performance in recruiting patients” across “numerous” studies and an existing “strong working relationship” with Parexel.
Patient recruitment
As the “UK’s largest recruiter and runner of commercial clinical trials across its UK sites”, Panthera has recently been the top recruiter globally in four studies, the top recruiter in the UK in six studies, and achieved first patient in globally or in the UK in nine studies. The company statement acknowledges that “less than 10%” of physicians and patients participate in clinical research. Among patients who do participate, “minority groups are significantly underrepresented”.
“Research activities are often concentrated in academic institutions and investigator sites, so patients and their providers are often unaware of the work, and even if they’re interested, many lack the time and resources required to join studies.”
Site Management Organisations (SMOs) like Panthera are focussed “entirely” on recruiting patients and running clinical trials, collaborating with local GP practices and using targeted advertising and social media campaigns to ensure that “all sections of the community” can participate.
Delivering efficiencies
The Parexel Site Alliance Network engages more than 340 sites and 16,000 investigators in “long-term collaborative relationships”. It is intended to “deliver efficiencies” to patients, sites, and customers. Members partner with Parexel to improve research and patient experiences.
Chris Dodd, Chief Commercial Officer at Panthera, described the company’s selection as a “testament to the effort we have put in to ensure we meet or exceed our patient recruitment targets”.
“We are delighted to be working in partnership with such a successful organisation with such great site communications and stakeholder management. We look forward to working together to bring even more clinical research to the UK.”
Join us at the Congress in Barcelona to explore ways in which the whole vaccine value chain can contribute to greater diversity in research and improved participant experiences. Don’t forget to subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Oct 15, 2024 | Global Health |
A study in Emerging Infectious Diseases explores the association between COVID-19 vaccination and facial palsy (FP) in South Korea. The authors use an immunisation registry linked to the national health information database to compare FP incidence in a risk window with a control window. They found an increased FP risk within 28 postvaccination, primarily after first and second doses of both mRNA and viral vaccines. They encourage clinicians to “carefully assess” the FP risk-benefit profile associated with COVID-19 vaccines and monitor neurologic signs after vaccination.
Risk of facial palsy
Although no severe safety concerns were observed during the clinical trials of COVID-19 vaccines, an “imbalance” in facial palsy (FP) incidence after vaccination was identified in vaccinated persons compared to the general population. The aetiology of FP “remains elusive”, but autoimmune mechanisms or vaccination are “considered potential contributors to its development”. FP is included in the priority list of adverse events of special interest generated by the Safety Platform for Emergency vACcines (SPEAC) because of its “sudden and acute symptom onset”.
Despite multiple studies on the association of FP with COVID-19, we lack a “clear consensus”. As these studies have produced “controversial and inconclusive results”, the authors identified a need to generate an “in-depth body of evidence and a clear consensus” on the subject.
The study
The study uses two large, linked databases in South Korea to conduct a self-controlled case series analysis. It is intended to provide evidence on the safety of COVID-19 vaccines for immunisation under the COVID-19 Vaccine Safety Research Committee (CoVaSC) in South Korea. Several vaccines were available during the study period in South Korea:
- BNT162b2 (Pfizer-BioNTech)
- mRNA-1273 (Moderna)
- ChAdOx1 nCoV-19 (AstraZeneca)
- Ad.26.COV2.S (Janssen)
- NVX-CoV2373 (Novavax)
The researchers identified persons aged 18 and older who received an initial COVID-19 vaccine dose between 26th February 2021 and 1st March 2022. Among this population, they identified and included patients with a primary FP diagnosis accompanied by a prescription for corticosteroids between 26th February 2021 and 31st October 2022; patients who had received a COVID-19 vaccination and had incident FP diagnosed within a prespecified observation period were also included.
Exclusion criteria included foreign born residents, participants in clinical trials, persons vaccinated abroad, and persons deviating from vaccination guidelines to account for potential exposure misclassification. Persons with a history of FP in the year preceding the observation period and those whose FP cases occurred after the end of the observation period were excluded.
44,564,345 persons in South Korea were administered 129,956,027 COVID-19 vaccines doses between 26th February 2021 and 1st March 2022. During the study period, 15,472 FP cases with corticosteroid prescriptions were identified. Among these, 5,211 occurred up to 28 days postvaccination: 4.0 GP cases/1 million doses. Among the FP study population, the mean age at first COVID-19 vaccination was 53.1 years. 54.7% were male and 45.3% were female.
The study showed FP risk increased within 1-28 days after any COVID-19 vaccine dose. Increased FP risks were observed with the second dose and combined first and second doses, but no association was found for the third dose. The increased FP risk was identified across vaccine types. The incidence rate ratios (IRR) were “generally consistent” across age groups and, after application of the Benjamini-Hochberg adjustment, “generally remained consistent” across sex.
Implications
The findings of this study add to growing evidence of a positive association between FP and COVID-19 vaccination. The exact biological mechanism for the development of FP after vaccination remains unknown. However, “plausible links” between FP and mRNA and viral vector vaccines have been proposed. The study revealed increased FP risk in persons homologously vaccinated with mRNA vaccines, especially for BNT162b2 and in those with at least a single dose of mRNA vaccine. Furthermore, it revealed elevated risks among patients who received homologous dosing of viral vector vaccines.
An important consideration is the suggested link between COVID-19 infection itself and FP onset. In South Korea, the annual incidence of Bell’s palsy increased from 23.0 to 30.8 cases per 100,000 persons from 2008 and 2018. It reached 32.5 cases per 100,000 persons during 2021-2022, which suggests an increasing trend during the pandemic. Additionally, a study in South Korea indicated that COVID-19 infection is associated with a higher risk for Bell’s palsy for both COVID-19 vaccine recipients and nonrecipients.
“In conclusion, our study revealed a transient risk for FP after any dose of COVID-19 vaccine.”
The authors note that, although the risk for FP “appears elevated”, the absolute number of cases was “small”. Risk for FP should therefore not discourage patients from receiving COVID-19 vaccinations.
“Because FP is generally mild and manageable, physicians should monitor neurologic signs after COVID-19 vaccination and provide patients with a comprehensive evaluation of the risk-benefit profile associated with COVID-19 vaccines.”
Join us at the Congress in Barcelona this month to explore the processes by which vaccine safety is evaluated and monitored after rollout, and don’t forget to subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Oct 14, 2024 | Global Health |
Phase II trials of a “promising” human vaccine candidate against Rift Valley fever are beginning in Kenya with CEPI support. CEPI reported in October 2024 that this is the “most advanced stage of testing” for a human Rift Valley fever vaccine in an “outbreak-prone area”. Scientists at the University of Oxford and the Kenya Medical Research Institute (KEMRI)-Wellcome Trust Research Programme are leading the trial with $3.7 million funding from CEPI.
Rift Valley fever
First identified in Kenya’s Rift Valley, Rift Valley fever is usually found in people after direct contact with infected animals or bites from infected mosquitoes. Most infected people experience “mild disease”, but a small proportion develop the “severe haemorrhagic form”, with a risk of blindness, convulsions, encephalitis, and bleeding. In these cases, mortality rates can reach 50%.
Rift Valley fever has been detected across “much of Africa” and in the Middle East. It is mosquito-borne, which makes it “climate sensitive”. There is therefore a risk of outbreaks spreading to new areas or increasing in frequency or size. There are Rift Valley fever vaccines for animals, but no currently available or licensed vaccines for human use; the disease is a priority disease for R&D for WHO and CEPI.
ChAdOx1 RVF in trial
The vaccine, known as ChAdOx1 RVF, is based on the University of Oxford’s ChAdOx1 vaccine platform. It has shown positive results in healthy adults in the UK, meeting “many of the optimal product characteristics” of a WHO target product profile. It is one of three Rift Valley fever candidates in CEPI’s portfolio. 240 healthy adults will participate in the research, following local trial approvals.
Funding for the trial comes under CEPI’s strategic partnership with the University to accelerate the development of globally accessible vaccines against outbreak pathogens. Both organisations are “committed to enabling access to any vaccine outputs developed through this partnership”, including developing a target product profile suitable for low- and middle-income countries (LMICs), assessing the need for technology transfer, and priority supply to LMICs at an affordable price.
Professor George Warimwe, Principal Investigator of the trail and Deputy Executive Director of the KEMRI-Wellcome Trust Research programme, reflected that “nearly 100 years” after the disease was identified, there are “still no approved vaccines or treatments”.
“This vaccine trial brings us closer to addressing the rising frequency of outbreaks.”
Dr Richard Hatchett, CEO of CEPI, commented that Rift Valley fever “disproportionately affects the lives and livelihoods of vulnerable pastoral communities”, causing human fatalities and livestock losses.
“Investing in the promising human ChAdOx1 RVF vaccine diversifies CEPI’s portfolio and gives us a greater chance at protecting vulnerable populations against this worrisome threat that may become more prevalent with climate change.”
Director General of Africa CDC, H.E. Dr Jean Kaseya, agreed that the disease “leads to livestock losses and human fatalities, thus impoverishing communities who largely depend on livestock for their livelihood”.
“The launch of a Phase II clinical trial of a Rift Valley fever vaccine candidate in an endemic country is a crucial milestone in our efforts to control this disease. Africa CDC is proud to support this initiative that not only prioritises the health of our people but also demonstrates the continent’s growing leadership in advancing clinical research.”
Dr Kaseya stated that the ChAdOx1 RVF vaccine “offers hope to vulnerable populations” who are “disproportionately affected by the growing impact of climate change”.
Join us at the Congress in Barcelona later this month to explore efforts to address the growing challenges of climate change and infectious disease with vaccine development and don’t forget to subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Oct 14, 2024 | Therapeutic |
Transgene announced in October 2024 that the primary objective of its randomised Phase II study of TG4001 has not been met. The study was evaluating TG4001 in combination with avelumab versus avelumab alone in patients with recurrent or metastatic HPV16-positive cervical and anogenital tumours. The primary objective was improvement in progression-free survival. Although this failure is “disappointing” to the company, Transgene states that it is evaluating the full results to “determine the best way forward”.
TG4001
Transgene’s TG4001 is an “innovative therapy capable of combating papillomavirus-induced cancers”. It teaches the immune system to identify and destroy the cancer cells expressing HPV-16 antigens, specifically E6 and E7.
Results and implications
The pre-planned subgroup analysis showed a positive efficacy trend in favour of the TG4001-containing regiment in cervical cancer patients. However, this requires further confirmation through additional analyses. These patients account for around half of the total patients enrolled in the study. Treatment was well tolerated, with adverse events “consistent” with previous observations.
“Transgene is currently evaluating the full study results in detail to determine the best way forward for this programme and will communicate further once this is completed.”
Dr Alessandro Riva, Chair and CEO of Transgene, acknowledged that “failure to meet the primary objective in our Phase II study with TG4001 is disappointing”.
“Nevertheless, we are encouraged by the positive efficacy trend in favour of the combination regiment in cervical cancer patients. We plan to complete a full and rigorous analysis of the data before deciding on any path forward for this asset.”
Dr Riva thanked patients and caregivers for their “important contribution” to the study.
“With a diversified portfolio of novel immunotherapies targeting solid tumours, our strategy remains focussed on advancing our lead asset, TG4050, an individualised cancer vaccine for head and neck cancers for use following surgery and adjuvant therapy.”
For the latest cancer vaccine research updates don’t forget to get your ticket to the Congress in Barcelona this month and subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Oct 11, 2024 | Technology |
CEPI announced in October 2024 that the Centre for Infectious Disease Research and Policy (CIDRAP) at the University of Minnesota is to receive US$3.2 million to advance its open access Coronavirus Vaccines Research and Development (R&D) Roadmap. This is an “important tool created to guide the development of vaccines” against multiple coronaviruses. CIDRAP will monitor and evaluate R&D progress and “catalyse efforts” to develop broadly protective vaccines. The investment from CEPI will monitor progress towards the roadmap goals and milestones and enable the creation of an online database of current literature and reports on coronavirus vaccine research.
The CIDRAP roadmap
CIDRAP’s roadmap is developed with guidance from over 50 scientific leaders and financial support from The Rockefeller and Gates Foundations. It aims to respond to the threat of coronaviruses, highlighted in the experience of three new coronavirus epidemics (SARS, MERS, COVID-19) in just 20 years. Coronaviruses are a “real and present threat” that demand a “large, comprehensive, and coordinated” initiative.
“The ultimate goal of developing broadly protective coronavirus vaccines is therefore multi-faceted: to create more efficacious and durable COVID-19 vaccines, mitigate the potential threat of future coronaviruses that have not yet emerged, and, ideally, prevent infections and transmission.”
The roadmap covers five topic areas each with “key barriers and knowledge gaps” and corresponding “technical milestones for measuring success”:
- Virology applicable to vaccine R&D
- Immunology and immune correlates of protection
- Vaccinology
- Animal and human infection models for coronavirus vaccine research
- Policy and financing
CEPI’s support
The funding contributes to monitoring progress on these goals and milestones and supports an open access online research database as well as an open access online summary of all broadly protective coronavirus vaccines in preclinical and clinical development and a dashboard tracking funding and investment.
Dr Michael Osterholm, Regents Professor and Director of CIDRAP recognised CEPI’s contribution to coronavirus vaccine research and development.
“CEPI’s support and collaboration with CIDRAP will fast forward our efforts at creating broadly protective coronavirus vaccines.”
Dr Kent Kester, Executive Director of Vaccine R&D, CEPI, commented that COVID-19 was the “third new coronavirus to strike in the past 20 years, portending the emergence of further novel coronaviruses”.
“Having the latest information on vaccine research and progress within coronavirus vaccine R&D readily and openly available in CIDRAP’s roadmap will enhance the approach being pursued by CEPI and other scientific investigators around the world to develop vaccines that could confer protection against multiple coronaviruses at the same time.”
For the latest coronavirus vaccine research updates, including insights into the challenges of universal vaccine development, join us at the Congress in Barcelona this month. Don’t forget to subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Oct 11, 2024 | Technology |
Orlance, Inc., announced in October 2024 that it has been awarded a National Institutions of Health (NIH) Fast Track Small Business Innovation Research (SBIR) grant to develop an Enhanced Seasonal Influenza Vaccine that provides “better protection against disease” even in years when there is a mismatch between predicted and actual circulating strains. The award includes $300,000 for Phase I; the total funding for the Phase I and II combined programme amounts to $3.3 million. The grant enables Orlance to leverage its innovative MACH-1 powdered vaccine and immunotherapy platform to address both seasonally changing and highly conserved influenza immunogens.
MACH-1 for influenza
MACH-1 is a high-performance microparticle ‘gene gun’ technology that “efficiently and uniquely” delivers DNA or RNA vaccine-coated microparticles into cells in the epidermis, which is “rich in immune stimulating cells”. An advantage of this technology in comparison with currently licensed mRNA vaccines is that MACH-1-delivered vaccines are stable at room temperature and are painless and needle-free. These vaccines also offer protective levels of immunity with the “smallest doses yet achieved within the field”.
The grant will enable a project to address the limitations of current flu vaccines by broadening the number of influenza strains targeted in one vaccine. This means vaccine production can occur closer to influenza season and achieve a better match between predicted and actual circulating strains. It will also stimulate “more diverse types of immune responses” in systemic and localised cells. The programme builds on Orlance’s universal influenza vaccine, adding seasonally changing influenza antigens to maximise protection.
Excelling in the field
Orlance’s Head of Research and Development and Principal Investigator Dr Kenneth Bagley commented on the importance of the MACH-1 technology.
“The unique properties of MACH-1 delivery into the highly immune competent epidermis that generates potent systemic and local respiratory mucosal antibody- and T cell-mediate immunity, coupled with the large payload capacity of DNA vaccines, may allow for Orlance’s universal influenza vaccine to excel where other universal vaccines have failed.”
Kristyn Aalto, CEO of Orlance, recognised the “continued funding support” from NIH.
“[The] support of the MACH-1 platform including this enhanced seasonal influenza vaccine reinforces the potential impact and significant step forward MACH-1 can bring to vaccine technology.”
We welcome Kristyn to the Congress in Barcelona this month for the Mucosal and Alternative Delivery workshop; get your tickets to join us for this here, and don’t forget to subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Oct 11, 2024 | Global Health |
A study in The Lancet in October 2024 finds that a single dose of typhoid conjugate vaccine (TCV) offers safe and effective protection against typhoid two years after vaccination in all children and sustained protection for older children at three to five years after vaccination. However, a “decline” in protection was observed after this period, with the greatest decline identified in children vaccinated at younger ages. The authors infer that a booster dose of TCV, perhaps around school entry age, might be needed for children vaccinated while younger than two years old, to sustain protection through the years when the risk is highest.
TCV
Typhoid fever places a “substantial disease burden” on low- and middle-income countries “marked by inadequate sanitation and limited access to clean water”. There are an estimated 7.15 million cases and 93,300 deaths each year. This burden is exacerbated by the “escalation” of antimicrobial resistance (AMR), which reduces treatment options. WHO recommends vaccines as an “important tool” in typhoid prevention and control strategies.
The first typhoid conjugate vaccine (TCV) was prequalified by WHO in 2017 based on field safety and immunogenicity data and findings from a controlled human infection model. 2-year vaccine efficacy has since been confirmed at 79-85% in randomised control trials. Research has revealed a “consistent trend” of waning protection in children vaccinated at a young age. Although WHO’s current recommendation is a single dose for infants and children from 6 months of age, epidemiological studies in countries across Asia and Africa suggest that incidence peaks in children between the ages of 5 and 9 years. Therefore, the authors identified a need to understand if a single dose of TCV can provide “substantial protection” in the medium and long term, or if a booster dose is needed.
Expanding the TyVAC trial: TyVOID
The cluster-randomise controlled trial (TyVAC) to assess the safety, immunogenicity, and protection conferred by a single dose of TCV started in Bangladesh in 2018 with a follow-up to 18 months. To generate further data, the authors extended this to evaluate vaccine protection and immunogenicity at 3-5 years after vaccination.
In TyVAC, healthy children aged 9 months to 15 years were offered TCV or a Japanese encephalitis vaccine according to their cluster of randomisation. 150 clusters were randomised to either TCV or the Japanese encephalitis vaccine, with 75 in each group. After a 3-month passive surveillance period, the baseline of TyVOID began at the final visit of TyVAC. Vaccinated children visited study clinics; after unmasking, participants in the Japanese encephalitis group were offered vaccination with a single dose of TCV, but TCV recipients were not offered the Japanese encephalitis vaccine.
Two cohorts of TCV-vaccinated children were available for follow-up:
- The group vaccinated in the original study between April 2018 and November 2019 (previous-TCV group)
- The group originally vaccinated with Japanese encephalitis and later TCV between January and August 2021 (recent-TCV group)
Results
During a median of 2.4 years, 14 episodes of typhoid fever were detected in the recent-TCV group (incidence rates of 31 per 100,000) and 45 episodes among the previous-TCV group (incidence rates of 97 per 100,000). The “significantly higher” incidence of typhoid fever in the previous-TCV group indicates a “drop in the vaccine effectiveness” 3-5 years after vaccination. The waning of vaccine effectiveness was further confirmed through the inclusion of unvaccinated children who sought care for fever as the reference group.
The decline in vaccine effectiveness correlated with age at vaccination; children in the youngest age group exhibited the most substantial reduction in vaccine effectiveness. The reason for the age-specific difference is “unclear”, but the authors suggest that underdeveloped bone marrow in younger children results in a weaker ability to support long-lived plasma cells. Another possibility is that older children have more opportunities for exposure to S Typhi than younger children, contributing to a greater durability of antibody concentrations after vaccination.
The issue of exposure is also relevant in comparing this study to a study in Malawi, as the incidence of typhoid fever in Bangladesh was “approximately three times higher”, with greatest disparity in younger children. Therefore, while a single dose of TCV might remain “highly effective” in Malawian children, it ceases to confer sufficient protection in Bangladeshi children.
“Put simply, it may be that more antibody is needed in Bangladesh to protect against typhoid fever than in Malawi as the incidence of infection is likely to be higher in Bangladesh.”
Implications
The introduction of TCV as a catch-up campaign in several countries is “likely to have a substantial impact” on the typhoid burden in these countries. TCV will then be integrated into local EPI programmes with a single dose, focussing on infants and toddlers. However, the authors urge WHO to evaluate their data and consider the “potential need for a booster around school entry age”.
Associate Professor Xinxue Liu of the Oxford Vaccine Group is one of the senior authors and emphasised how “serious and life-threatening” the disease is, particularly for “children and adolescents in low- and middle-income countries”.
“TCV offers the best chance to reduce the burden of typhoid, helping to reduce transmission and limiting further evolution of drug-resistant strains. This study provides additional information for policy makers on longer-term TCV protection and the importance of continued investigation and updated guidance.”
Dr Firdausi Qadri, Senior Scientist at the Infectious Diseases Division at the International Centre for Diarrhoeal Disease Research, Bangladesh (icddr,b) and first author, commented that the results “indicate a decay in antibody concentrations in different age groups”.
“[They] suggest that a booster dose around school entry age for children vaccinated while younger than 2 years could be considered, to sustain the protection from TCV through the school years when children are at greatest risk of typhoid.”
Professor Sir Andrew Pollard, Director of the Oxford Vaccine Group, reflected on WHO’s “current” recommendation.
“Epidemiological studies in different countries across Asia and Africa showed that the incidence of typhoid fever is much higher in children younger than 16 years than it is in adults, with the peak of cases seen in those aged 5-9 years. Whether a single dose of TCV provides long-term protection continues to be a top research priority to advise policy makers.”
For the latest vaccine research updates, why not subscribe to our weekly newsletters here? We hope you will also join us at the Congress in Barcelona this month to discuss vaccine questions and explore global health concerns.

by Charlotte Kilpatrick | Oct 11, 2024 | Global Health |
A WHO report in October 2024 suggests that vaccines against 24 pathogens could reduce the number of antibiotics needed by 22% every year. Some of these vaccines are already available but currently underused, but others will need to be developed and brought to market. The report expands on a WHO study from 2023, estimating that some vaccines already in use could avert up to 106,000 deaths caused by AMR each year. Director-General Dr Tedros Adhanom Ghebreyesus highlighted that addressing AMR “starts with preventing infections”, for which vaccines are “among the most powerful tools”.
“Prevention is better than cure and increasing access to existing vaccines and developing new ones for critical diseases, like tuberculosis, is critical to saving lives and turning the tide on AMR.”
The burden of AMR
Antimicrobial resistance (AMR) is the result of bacteria, viruses, fungi, and parasites changing to stop responding to medicines. As medicines become ineffective, infections become harder to treat, which increases the risk of disease spread, severe illness, disability, and death. The report introduces the significant global burden of AMR. In 2019, an estimated 7.7 million deaths were associated with 33 bacterial infections, with almost 5 million of these associated with AMR.
The mortality burden of these drug-resistant infections is “most pronounced” on the African continent, followed by South-East Asia and Eastern Europe. However, community mobility increases the risk of transmission to other continents. AMR has the potential to impose an annual global cost of up US$3.4 trillion by 2030, with the most severe consequences for low- and middle-income countries (LMICs).
A “key driver’ of AMR is the “systematic misuse and overuse” of antimicrobials in healthcare, animal health, and agriculture; the greatest contributor to overall use of antimicrobials is use in animals. The World Organisation for Animal Health (WOAH) estimated that 84,500 tonnes of antimicrobials were used in the animal sector in 2019. However, this is a 13% decrease from 2017. On the other hand, global antibiotic consumption in humans increase by 65% between 2000 and 2015 and is projected to triple (from 2015) by 2030.
One of the major challenges is ensuring equitable access to antimicrobials, particularly in LMICs, where “people are more at risk of dying from a lack of access to appropriate antimicrobials than from resistant infections”. Managing AMR demands both sector-specific and “One Health” approaches. Vaccines can be critical to efforts to lower the burden by reducing the incidence of drug-sensitive and drug-resistant infections, antibiotic use, and opportunities for evolution and transmission of resistant genes and pathogens.
The report
Although we know that vaccines are important aspects of the solution, their specific role in reducing AMR has not been “systematically evaluated and quantified”. Therefore, the latest report evaluates this and provides recommendations for “enhancing the impact of vaccines on AMR”. It covers 44 vaccines targeting 24 pathogens, drawing the characteristics of each vaccine from various sources. Three criteria were considered:
- The AMR-related health burden – measured by the reduction in deaths and DALYs associated with AMR
- Antibiotic use (or antimicrobial use in the case of Mycobacterium tuberculosis)
- The economic burden of AMR, including hospital costs and productivity losses
Highlights from the report
- Vaccines against 16 bacterial pathogens may prevent 510,000 deaths and 28 million DALYs associated with AMR.
- This prediction increases to include an additional 1.2 million deaths and 37 million DALYs when the use of vaccines is expanded to target all populations at risk of infection.
- The non-serotypespecific vaccine against S. pneumoniae, with increased efficacy against lower respiratory tract infections, would have the highest impact on both AMR-associated deaths and DALYs.
- The greatest impact of vaccines on reducing the burden of bacterial AMR in 2019 was in the WHO African Region, averting an estimated 170,000 deaths and 12 million DALYs annually.
- In the WHO South-East Asia Region, vaccines were estimated to have prevented 160,000 deaths and 7.5 million DALYs annually.
- The development and optimal use of vaccines against 23 pathogens could avert up to 2.5 billion defined daily doses a year, which is 22% of the global estimated antibiotic use in humans associated with treating these pathogens.
What’s next?
The authors suggest that the role of vaccines in addressing AMR is “often overlooked” in policy and decision-making processes. They highlight the need for “greater recognition and integration” of vaccines into AMR mitigation strategies and the importance of considering AMR in vaccine decision-making.
“To achieve appropriate inclusion of vaccines in the AMR agenda, the immunisation and AMR communities must strengthen their joint understanding of the evidence and enhance collaboration.”
How do you think that AMR priorities can be incorporated into vaccine development and deployment efforts? Join us for the AMR and bacterial vaccines track at the Congress in Barcelona this month to contribute to these conversations, and don’t forget to subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Oct 9, 2024 | Global Health |
GSK announced in October 2024 that data from the AreSVI-006 (Adult Respiratory Syncytial Virus) Phase III trial of Arexvy indicate that a single dose could offer protection for three RSV seasons. Arexvy is the world’s first RSV vaccine, first approved by the United States FDA in May 2023 for the prevention of lower respiratory tract disease (LRTD) caused by RSV in older adults. The latest trial evaluates the efficacy of a single dose of the recombinant, adjuvanted vaccine against LRTD caused by RSV in adults aged 60 years and older.
RSV is a “common contagious virus” that affects an estimated 64 million people of all ages globally each year. Adults can be at increased risk for RSV disease due to comorbidities, immune compromised status, or advanced age. RSV causes over 465,000 hospitalisations and 33,000 deaths in adults aged 60 and older in high-income countries.
Clinically meaningful efficacy
The results suggest that after a single dose of the vaccine, cumulative efficacy over three full RSV seasons was clinically meaningful at 62.9% against RSV-LRTD and 67.4% against severe RSV-LRTD compared to placebo. In the third season, vaccine efficacy was 48.0% against RSV-LRTD. The data include efficacy against different RSV subtypes, in adults between 70 and 79 years of age, and those with underlying medical conditions.
“Since RSV can exacerbate medical conditions and potentially lead to hospitalisations, cumulative efficacy over three RSV seasons has the potential for significant health impact.”
Another benefit of this protection is that healthcare professionals might have flexibility to administer the vaccine year-round. Over time, revaccination is “expected to be required to maintain an optimal level of protection”. Therefore, GSK will continue to share efficacy and immune response data to inform decisions on immunisation schedules and future revaccination.
GSK’s Chief Scientific Officer Dr Tony Wood is excited by the data, which show that a single dose could “help protect millions of older adults” to “benefit public health”.
“This is the only RSV vaccine with efficacy and safety data available through three full seasons. We will continue to provide data on longer term follow-up to help recommending bodies determine future revaccination schedules.”
We look forward to hearing from senior representatives of GSK, including for perspectives on directing vaccine development for older populations, at the Congress in Barcelona this month. Get your tickets to join us here, and don’t forget to subscribe to our weekly newsletters here!

by Charlotte Kilpatrick | Oct 8, 2024 | Therapeutic |
A study in the Journal for ImmunoTherapy of Cancer finds that vaccination in a clinically relevant genetic cancer mouse model generated a population of functional progenitor tumour-specific CD8 T cells (TST) and halted cancer progression, in contrast to immune checkpoint blockade (IBT) therapies. The authors hope that immunisation could be the “most effective strategy” for patients with early cancers or at high risk of cancer recurrence. This study takes a different approach to many cancer vaccine studies, which tend to focus on patients with advanced tumours.
Cancer vaccine potential
The authors recognise the transformational role of immunotherapies in the cancer treatment landscape, particularly in the case of immune checkpoint blockade (ICB). However, vaccines for non-viral cancers have had “more limited success”. Many studies on tumour-specific CD8 T cell (TST) vaccine responses are conducted in the established/late tumour setting, so less is known about how TST “respond and differentiate” in response to immunotherapy during early stages of tumorigenesis.
Previously, the authors developed an autochthonous mouse model of liver cancer (AST;Cre-ERT2) to initiate liver carcinogenesis with tamoxifen (TAM)-induced Cre-mediated SV40 large T antigen (TAG) expression in hepatocytes. TAG functions as an oncogene and a tumour-specific neoantigen recognised by CD8 T cells, so the model enables “precise temporal control” of the duration of TST interactions with transformed hepatocytes and tumours. In contrast to human tumours, which “arise sporadically and progress clonally”, TAM-induced oncogene induction is “highly efficient”, resulting in high antigen burden even at early stages.
The study
The researchers allowed AST;Cre-ERT2 mice to undergo stochastic TAG oncogene activation through sporadic, TAM-independent Cre-mediated activity. To explore TST responses against TAG-driven tumours they used congenic donor lymphocytes from transgenic mice, in which CD8 T cells express a single T cell receptor (TCR) specific for TAG epitope-I (TCRTAG). They found that TST became dysfunctional in TAM-treated AST;Cre-ERT2 mice and were “unable to halt tumour progression”. TAM-treated AST;Cre-ERT2 mice had a “substantial” tumour antigen burden, even at early stages of tumorigenesis.
To compare initial TST differentiation in mice with early liver lesions against those with late liver lesions, the researchers transferred CFSE-labelled naïve TCRTAG into early and late time point AST;Cre-ERT2 mice. TCRTAG in mice with early lesions divided at a slower rate, particularly in the spleen and ldLN, and there were fewer TCRTAG in the spleens, ldLN, and livers of early mice. Decreased TST proliferation in mice with early lesions could be due to the lower TAG antigen burden. Although nearly all TCRTAG in mice with late lesions and most in mice with early lesions failed to produce effector cytokines TNFα and IFNγ within 60 hours of transfer, a population of TCRTAG in were identified in the spleen and liver of mice with early lesions. These could produce effector cytokines TNFα and IFNγ.
“Thus, in hosts with sporadic early lesions, a subset of TST resisted rapid differentiation to the dysfunctional state, raising the possibility that this subset might be amenable to immunotherapeutic reprogramming/rescue.”
To see if this functional TST subset persisted, the authors examined TCRTAG immunophenotype and function 5 days and 21 days post-transfer into early or late AST;Cre-ERT2 mice. While fewer TCRTAG were found in mice with early lesions compared to late lesions at 5 days, the difference became less pronounced at 21 days. In both groups TCRTAG upregulated CD44, which indicates antigen exposure and activation. TCRTAG in early mice continued to express higher levels of PD1 than naïve TCRTAG, suggesting that PD1 expression can identify tumour-reactive TST in hosts with early lesions.
The next consideration was if the functional TST subset in mice with early lesions could be harnessed to stop tumour progression. LM, a gram-positive intracellular bacterium, induces strong CD4 and CD8 T cell responses. The researchers used an actA inIB deficient attenuated LM vaccination strain to test if early vaccination of AST;Cre-ERT2 would protect mice against liver cancer progression. Mice were either left untreated, given a single dose of empty LM, or vaccinated with a single dose of LM- TAG.
“LM- TAG–immunisation conferred a major survival advantage, with all mice remaining tumour-free and one mouse euthanised for dermatitis without any evidence of liver tumours.”
The mice in untreated and empty LM groups reached endpoint with “multiple” large liver tumours and increased liver weight. At endpoint, most TCRTAG in the LM- TAG–immunised made effector cytokines, in contrast to the TCRTAG in tumour-bearing mice in the other groups, which were “largely unable to produce effector cytokines”.
Vaccination vs ICB
“An important and open question in cancer immunotherapy is how ICB versus vaccination compares in boosting anticancer immune responses, and how best to combine and sequence these therapies.”
A comparison of ICB, LMTAG vaccination, and combined ICB/LMTAG vaccination found that ICB conferred no benefit in comparison with isotype control antibodies (iso). By contrast, LMTAG and ICB/LMTAG treated mice had no evidence of tumour progression at 400+ days. Furthermore, LMTAG vaccination, whether alone or in combination, led to a “substantial increase” in TST numbers and IFNγ production, while ICB alone had “little impact”.
LM-based vaccines have had “poor or mixed results” in clinical trials, often with a target of patients with advanced or refractory cancers. The authors hope that their studies offer “mechanistic insight” as to why these fail in patients with advanced cancers: “for vaccines to be effective, a progenitor TST population must be present”. Although the apparent superiority of vaccination over ICB “may be surprising at first glance”, the authors highlight an important point, that “not all TCF1+TST are functional, nor does ICB alone lead to functional TST”. However, the findings suggest that LMTAG vaccination maintains or rescues functional progenitor TCF1+TST.
Timing is important
Dr Mary Philip, associate director of the Vanderbilt Institute for Infection, Immunology, and Inflammation, commented that the study “suggests that the timing of vaccination is important”.
“A unique feature of our study is that these mice are at high, essentially 100% risk of developing cancers, so the fact that a single immunisation at the right time can give lifelong protection is pretty striking.”
Dr Philip reflected that very few studies follow mice “so long after vaccination” and find them tumour free for two years.
“ICB works by taking the brakes off T cells, but if the T cells have never been properly activated, they are like cars without gas, and ICB doesn’t work. The vaccination boosts the T cells into a functional state so that they can eliminate early cancer cells.”
For more progress updates from cancer vaccine researchers at the Congress in Barcelona this month, get your tickets to join us here. Don’t forget to subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Oct 7, 2024 | Global Health |
A week after the declaration of a Marburg outbreak in Rwanda in September 2024, Sabin Vaccine Institute announced that it is providing doses of its investigational Marburg vaccine to support the outbreak response. An initial shipment of approximately 700 doses will be used in a trial involving frontline workers, including healthcare professionals, who have been the “hardest hit” by this outbreak. Sabin and the Rwanda Biomedical Centre have entered a clinical trial agreement for a Phase II rapid response open label study, which will be conducted at six trial sites in Rwanda. Sabin also plans to supply additional vaccines, pending a request from Rwandan officials and authorisation from BARDA.
Responding to the outbreak
The outbreak was declared on 27th September 2024, and by 6th October it had caused 12 deaths. Many cases are among health workers in two facilities in Kigali, but there are more cases spread across other districts. Sabin has been “working directly” with Rwandan officials and partners to support the response. There are no licensed vaccines or treatments for Marburg, but Sabin’s single-dose vaccine is in Phase II trials in Uganda and Kenya, with no safety concerns reported to date. The vaccine is based on the ChAd3 platform and results from Phase I clinical trials and nonclinical studies suggest that it is safe and elicits “rapid” and “robust” immune responses.
Commenting on the support from Sabin, Rwanda’s Minister of Health Dr Sabin Nsanzimana reflected that “in emergency situations, the success of clinical trials relies on quick, strategic global partnerships” that combine “expertise, resources, and innovation”.
“Today, a week after this Marburg outbreak was first confirmed, we are receiving doses of the Sabin Vaccine Institute’s Marburg vaccine candidate to protect our health workers and other high-risk groups, and also advance scientific tools which will ensure this virus can be effectively controlled now and in the future.”
Lightning speed
Sabin’s Chief Executive Officer Amy Finan described the team’s “lightning speed” in responding to the Rwandan government’s request for assistance, preparing shipments, finalising protocols, and securing regulatory and legal approvals.
“This swift emergency response demonstrates that a dedicated, collaborative group of individuals and organisations can achieve remarkable results when united by a common cause: to contain a lethal disease outbreak and prevent further loss of life.”
ReiThera, Sabin’s manufacturing partner, has produced the drug substance and filled and finished doses for shipment. CEO Stefano Colloca stated that the ReiThera team believes in the “transformative power of global collaboration to advance science and create lasting impact”.
“Our partnership with Sabin highlights our shared commitment to developing a life-saving vaccine against Marburg disease with a mutual goal: to save lives and ensure that even the most vulnerable communities around the world have access to vital and equitable protection.”
Sabin’s vaccine progress
Sabin plans to launch a Phase II trial of the Marburg candidate in the United States next year, as it looks forward to interim results from the trial in Uganda and Kenya. The development programme is supported by BARDA, which has committed $235 million for advancing vaccine research and development against Sudan ebolavirus and Marburg virus diseases.
To join discussions about safety and effectiveness evaluations of vaccines deployed in emergency situations, get your tickets to the Congress in Barcelona this month. Don’t forget to subscribe to our weekly newsletters for vaccine updates.

by Charlotte Kilpatrick | Oct 4, 2024 | Technology |
In September 2024, Vaxart announced the initiation of the sentinel cohort of its Phase IIb clinical trial evaluating the oral pill COVID-19 vaccine candidate in comparison with an approved mRNA vaccine. The funding is now approved for this part comprising 400 participants; 200 will receive Vaxart’s COVID-19 vaccine candidate and 200 will receive the approved mRNA vaccine comparator. The full trial will measure efficacy for symptomatic and asymptomatic disease, systemic and mucosal immune induction, and the incidence of adverse events.
Changing the vaccine landscape
Vaxart states that “for two hundred years vaccines have been administered by intramuscular injection”, offering the company’s oral pill vaccines as a way to “change everything”. The COVID-19 vaccine attacks invading pathogens at their points of entry, triggering strong IgA and T-cell responses to “repel and overwhelm” the invaders. It is designed to be stable at room temperature to allow global distribution with “wide public acceptance, minimal cost, and maximum speed”.
In trial
The Phase IIb trial has two parts and will enrol healthy adults in the United States. The first part will engage 400 participants; once an independent Data and Safety Monitoring Board (DSMB) and FDA review the data from these participants, the second part will be initiated, enrolling 10,000 participants. A goal of the trial is to enrol participants “in line with U.S. demographics”, and to include at least 25% over the age of 65.
The primary endpoint is relative efficacy of Vaxart’s candidate compared to the approved mRNA vaccine for the prevention of symptomatic disease. Primary efficacy analysis will be performed after all participants have either discontinued or completed a study visit 12 months after vaccination. Funding was granted through BARDA’s Project NextGen initiative to accelerate and streamline the development of innovative COVID-19 interventions, including vaccines.
A strong step
Dr James Cummings, Vaxart’s Chief Medical Officer, described the initiation of the sentinel cohort as a “strong step” towards the goal of “developing a vaccine that may bring us closer to a sustainable solution to the persistent threat of COVID-19″.
“We continue to progress toward our goal of conducting the Phase IIb study and look forward to the results of our mucosal technology’s first head-to-head comparison against an approved mRNA vaccine for this virus.”
We look forward to learning more about the vaccine’s progress from Dr Cummings at the Congress in Barcelona this month; if you’d like to join us there do get your tickets now. Don’t forget to subscribe to our weekly newsletters for more updates!

by Charlotte Kilpatrick | Oct 4, 2024 | Global Health |
The University of Oxford announced in October 2024 that scientists working on ‘OvarianVax’ a vaccine to encourage the immune system to “recognise and attack” the earliest stages of ovarian cancer, have secured funding from Cancer Research UK. The team will receive up to £600,000 over the next three years to support research from establishing targets to possible clinical trials. Although getting a vaccine to the point where it is “widely available to women at risk of ovarian cancer” is “many years” away, the funding is an “exciting step” towards preventing ovarian cancer at an early stage, rather than treating it after it has taken hold.
Ovarian cancer
Ovarian cancer is the 6th most common cancer in women, causing around 7,500 new cases every year in the UK. There is currently no screening programme for the disease, and some women with are at higher risk with inherited copies of altered genes. Compared to women without gene alterations, women with altered BRCA1 genes face a higher risk by up to 65%, and women with altered BRCA2 genes face a higher risk by up to 35%.
Women with these alterations are recommended to have their ovaries removed by the age of 35, which has implications for having children and brings on early menopause. Many cases of ovarian cancer are only identified at a late stage. Professor Ahmed Ahmed is the Director of the Ovarian Cancer Cell Laboratory, MRC Weatherall Institute of Molecular Medicine at the University of Oxford, and lead for the OvarianVax project and comments that “we need better strategies to prevent ovarian cancer”.
“Currently women with BRCA1/2 mutations, who are at very high risk, are offered surgery which prevents cancer but robs them of the chance to have children afterwards.”
However, a possible “solution” could be on the horizon with the OvarianVax project, focussed on women at high risk but with potential to expand if trials are successful.
“Thanks to this funding, our research can take a big step forward towards a viable vaccine for ovarian cancer.”
Vaccine development
The researchers will identify the proteins on the surface of early-stage ovarian cancer cells that are most strongly recognised by the immune system and work out how effectively the vaccine kills organoids, “mini-models” of ovarian cancer. If this proves successful, they will move forward to clinical trials in the hope that one day women could be offered the vaccine to prevent ovarian cancer.
“Teaching the immune system to recognise the very early signs of cancer is a tough challenge. But we now have highly sophisticated tools which give us real insights into how the immune system recognises ovarian cancer.”
Professor Ahmed’s team has already found that immune cells from patients with ovarian cancer can “remember” the tumour. They will use this discovery to train the immune system to recognise over 100 proteins on the surface of ovarian cancer, known as tumour-associated antigens. The research will uncover which antigens trigger the immune system to recognise and kills cells that are becoming ovarian cancer, using tissue samples from the ovaries and fallopian tubes of people with ovarian cancer to recreate the early stages of disease.
The team will also work with patient and public representatives to understand who would be willing to take the vaccine, who would receive the most benefit from it, how it could be administered, and how to ensure it is taken up by as many eligible women as possible if it is successful in clinical trials.
Prevention research strategy
This is one of several projects that Cancer Research UK is funding within its prevention research strategy, which seeks to use discoveries from the lab to find more precise ways to prevent cancer. Cancer Research UK’s Chief Executive, Michelle Mitchell, described these projects as “a really important step forward into an exciting future, where cancer is much more preventable”. The funding should “power crucial discoveries” that can be used to “realise our ambitions to improve ovarian cancer survival”.
“OvarianVax builds on the exciting developments in vaccine technology during the pandemic. This is one of the many projects which we hope will give women longer, better lives, free from the fear of cancer.”
For more on using the latest lab discoveries to improve patient outcomes with vaccines, get your tickets to the Congress in Barcelona this month, and don’t forget to subscribe to our weekly newsletters here.

by Charlotte Kilpatrick | Oct 2, 2024 | Global Health |
In October 2024, CEPI announced the expansion of research into Lassa fever in West Africa in a “pioneering study” to explore the variation in disease symptoms and how this compares to other “worrisome infections” in the region. The project, led by the Nigeria Centre for Disease Control and local study sites, comes under the Enable study, created by CEPI and partners to provide a more accurate picture of the disease burden in West Africa and help inform outbreak preparedness efforts, including Lassa vaccine development. Lassa fever, a known public health burden in the region, infects “hundreds of thousands” every year. However, cases are likely underreported due to detection difficulties.
Lassa fever
Although it was described in the 1950s, the virus causing Lassa fever was only identified in 1969. It is a single-stranded RNA virus in the Arenaviridae family. The disease is a “potentially deadly haemorrhagic illness” with an estimated 1% case fatality rate. Most infections are thought to be “minimally symptomatic or asymptomatic”, which means they avoid detection. People who do experience symptoms can suffer fever, headache, and chills, and could be misdiagnosed with diseases like Ebola, dengue, or malaria.
As a WHO priority disease, Lassa fever is in “urgent need” of research and development. Understanding the disease is critical to vaccine development, which Dr Muhammad Ali Pate, Coordinating Minister of Health and Social Welfare of Nigeria, recognises.
“Lassa fever remains a public health burden in Nigeria and West Africa, but the commitment to research and innovation is yielding promising progress. The new Enable research will deepen our understanding of the virus and enhance the work being undertaken to develop the first-ever Lassa vaccine to safeguard the health of our communities.”
Dr Pate highlighted the Ministry’s commitment to collaboration to “advance these efforts and bring the suffering caused by Lassa fever to an end”.
Enable expanded
Enable was launched in 2019, and in 2021 CEPI announced funding to provide a “more accurate assessment” of the incidence of Lassa fever infections. CEPI offered US$ 10.3 million to partners in Benin, Guinea, Liberia, and Sierra Leone to participate, enrolling up to 23,000 participants to understand the “rate, location, and spread of Lassa virus across the region”. The results are also central to CEPI’s goal of producing a licensed Lassa vaccine.
The new year-long study will invite 5,000 healthy people, including children and infants, to participate at sites in Nigeria (Edo, Ondo, and Ebonyi states), Sierra Leone, and Liberia. It is intended to improve understanding on how commonly the disease occurs, how rates of infection and symptoms vary across locations, ages, sex, and exposure history, and the extent of post-infection symptoms. Scientists will also explore how often people are co-infected with Lassa fever and malaria, as co-infections may complicate the clinical course of each disease.
Vaccine goals
Dr Richard Hatchett, CEO of CEPI, explained that “incomplete detection” of cases affects both the understanding of the true incidence rate and level of response, but could also “threaten the evaluation, rollout, and acceptance of future Lassa vaccines”.
“Insights gained on the diversity of disease symptoms will enhance our understanding of Lassa fever, categorised into mild, moderate, or severe cases. This information will be crucial in guiding where and how future late-stage vaccine trials are conducted and determining priority groups for receiving the Lassa vaccine once it becomes licensed in the coming years.”
A 2024 modelling study found that around 3,300 lives could be saved over 10 years with a Lassa vaccine. It could also avert up to $128 million in societal costs. The most advanced vaccine candidate is developed by IAVI and is currently in Phase II trials in the region. Enable National Project Coordinator in Nigeria, Mrs Elsie Ilori, described the launch of the expanded study as a “key step in our ongoing efforts to understand and combat this dreadful disease”.
“Through deeper investigations into the variations of Lassa fever symptoms and their comparison to other infections within the region, we will obtain valuable insights that can improve diagnosis, boost outbreak preparedness, and inform the future vaccine development.”
Dr Jilde Idris, Director General of Nigeria Centre for Disease Control and co-chair of the Nigeria Lassa Vaccine Task Force agreed that the investigation “represents key progress in our battle against Lassa fever”.
“We are improving our capacity to identify and recognise cases while preparing for future vaccine development by examining the disease’s symptoms and its connection to other infections.”
The work is “vital for forming health practices” and “promoting” public health in the region, and Dr Idris welcomed the support of partners and local communities in “making strides towards lessening the impact of Lassa fever” and preparing for a “future that can block its life-threatening effects”.
For more on IAVI’s vaccine efforts and insights into challenge studies in West Africa, join us at the Congress in Barcelona this month for a session with Dr Marion Gruber. Don’t forget to subscribe to our weekly newsletters here for vaccine updates!

by Charlotte Kilpatrick | Oct 2, 2024 | Therapeutic |
Interim Phase II data from Gritstone bio’s study evaluating GRANITE in September 2024 are described as “encouraging” in a company statement. The study evaluates Gritstone’s individualised neoantigen targeting immunotherapy in frontline microsatellite stable colorectal cancer (MSS-CRC) as maintenance therapy in combination with immune checkpoint inhibitors and fluoropyrimidine/bevacizumab. These data show the vaccine’s potential to extend progression-free and overall survival, but “fell short” of the target that some suggest is needed to “transform its fortunes”.
Encouraging data
104 patients were randomised 1:1 in the study, and the treated analysis shared by Gritstone includes 69 patients. Highlights from the data include:
- An emerging progression-free survival (PFS) benefit to all GRANITE recipients
- 21% relative risk reduction of progression or death with GRANITE compared to standard of care (SOC) control in all treated population
- 33% of GRANITE and 23% of control patients remain on study and free of progression
- Clinical benefit was most notable in patients with low disease burden (defined as patients with circulating tumour DNA (ctDNA) equal to or below the trial population median value at study entry)
- 38% relative risk reduction of progression or death with GRANITE compared to SOC control with low ctDNA subgroup
- Low baseline ctDNA is a likely prognostic and predictive factor
- Immune data were consistent with clinical activity
- Functional neoantigen-specific T cells observed in all 16/16 GRANITE patients tested by ELISPOT
- Association of PFS and peak ex vivo ELISPOT responses was apparent, indicating that ex vivo ELISPOT may be a surrogate for PFS
- GRANITE demonstrated a favourable safety and tolerability profile
- No patients discontinued study treatment due to an adverse event (AE)
- Common AEs were the mild systemic and local effects associated with any potent vaccine
- One treatment-related serious AE (fatigue) occurred in the GRANITE arm but patient continued GRANITE treatment without recurrence upon recovery
Gritstone recognises a need for continued follow-up to “fully assess” the effects of GRANITE and determine whether a plateau of improved PFS, which indicates durable clinical benefit, is achieved. Gritstone bio’s co-founder, President, and CEO Dr Andrew Allen is “excited by the potential” seen in GRANITE to extend both progression-free and overall survival “in a disease where relentless progression is the rule with existing therapies”.
“The field of neoantigen-targeting immunotherapy is evolving rapidly, and the focus is shifting to patients with lower volume disease. Notably, patients with newly diagnosed metastatic disease who have lower ctDNA at study entry and thereby relatively low disease burden, could benefit from this type of immunotherapy.”
More time needed
Dr Allen commented that “typically”, success for immunotherapy “manifests as an elevated plateau in PFS and overall survival Kaplan-Meier curves, and we may be seeing this in our low disease burden population.”
“We need more time to let these data mature.”
The “low and stable” ctDNA measurements in “most” GRANITE patients are “encouraging”, says Dr Allen, as that pattern is “not typically seen in patients about to develop disease progression”. There is also “opportunity for greater effects in tumours more typically amenable to immunotherapy” in the potential benefit observed in MSS-CRC, a “notoriously ‘cold’ tumour”.
“These data support further exploration of GRANITE in frontline MSS-CRC and in other low burden (neo)adjuvant settings. With this new dataset in hand, we continue to actively explore several strategic and funding alternatives to rapidly advance our innovative immunotherapy for the benefit of patients.”
Head above water
The company statement also confirmed that Gritstone has engaged a financial advisor to support its exploration and review of potential “value-maximising strategies”. While Gritstone “does not intend to discuss or disclose further developments”, speculation continues.
Evercore ISI analyst Jonathan Miller is quoted by Fierce Biotech wondering if the company’s cash runway is “functionally no later than” the end of the year. Although “on the face of it” the progress is positive, the data have “limitations”, such as a shift away from patients with more aggressive disease. Miller believes that if Gritstone can keep tracking patients, the extend follow up can continue to look encouraging, but questions the company’s future.
“They don’t have flexibility to run this data out much further, add [patients], or explore [the] adjuvant setting.”
We look forward to welcoming Gritstone’s EVP and Head of R&D, Dr Karin Jooss, to the Congress in Barcelona this month, to share insights in the Cancer and Therapeutic Vaccines track. Get your tickets to join us here, and don’t forget to subscribe to our weekly newsletters for the latest vaccine news.